Psoriatic arthritis belongs to an umbrella group termed as ‘spondyloarthritis’ (SpA), which is used to describe a group of inter-related disorders. As a group, they share the following distinctive clinical, radiologic and genetic features: Axial joint involvement; peripheral joint disease; familial clustering, presence of HLA-B27; extra-articular features (in particular uveitis, inflammatory bowel disease); and enthesopathy. Based on these features, it is obvious that SpA is markedly distinct from rheumatoid arthritis (RA). Although ankylosing spondylitis (AS) is the prototype of this particular group, this group consists of several disorders: Reactive arthritis; psoriatic arthritis (PsA); arthritis related to inflammatory bowel disease (ie, Crohn’s disease and ulcerative colitis); and a subgroup of juvenile idiopathic arthritis (JIA).
Inflammatory arthritis associated with psoriasis has long been recognised. Its identity as a separate form of arthritis faced initial controversy, and it was debated whether it represents a separate disease entity or simply the co-existence of RA and psoriasis.
However, the discovery of rheumatoid factor in 1948 paved the way towards its recognition as a clinical entity separate from RA. PsA was formally recognised as a separate disease by the American Rheumatism Association (now the American College of Rheumatology) in 1964, and it is now recognised as one of the forms of seronegative inflammatory spondyloarthritis. PsA was initially defined by Moll and Wright as “an inflammatory arthritis in the presence of psoriasis with a usual absence of rheumatoid factor”.
To date, there has been mounting evidence that this disease is distinct from RA and other spondyloarthropathies, and this is based on data derived from characteristic clinical features, histopathologic analyses, immunogenetic associations and musculoskeletal imaging.
Although once considered a milder form of arthritis, it is now well established that PsA can cause significant joint damage. Research has shown that among 220 patients with PsA, deformity, radiological damage, or both, was present in more than five joints in about 16 per cent of the patients.
Moreover, 67 per cent of these patients had erosive joint disease. Similarly, an inception cohort study has shown that 47 per cent of the PsA patients who presented within five months of onset of symptoms had ≥1 erosion by the second year of follow-up, despite the fact that the majority had been treated with disease-modifying anti-rheumatic drugs (DMARDs).
There are varied reports of its prevalence among patients with psoriasis, with the prevalence rates ranging from six-to-42 per cent.
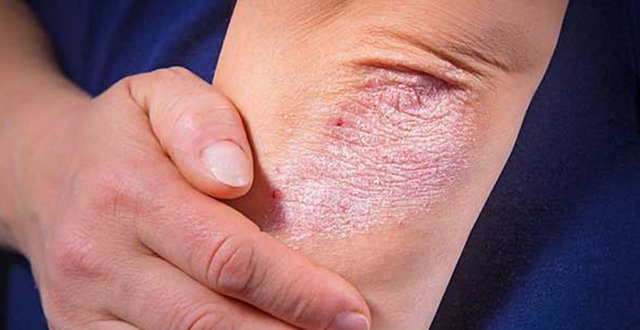
The severity of skin psoriasis is a poor clinical predictor of the development and severity of PsA. Psoriasis can be divided into type 1 and type 2, depending on the age at onset. Type-1 PsO begins at a young age (≤40 years), has a stronger family history, and is associated with certain HLA types. About 65 per cent of people with psoriasis have type-1 PsO. Type-2 PsO occurs in those >40 years old. Family history of psoriasis in such cases is weak or absent and it is generally not associated with HLA antigens.
<h3><strong>Clinical features</strong></h3>
Being a progressive inflammatory joint condition, PsA usually causes pain and joint damage, eventually leading to disability. The following are typical clinical symptoms of PsA involving different joints and their related compartments, which are being better defined as distinctive characteristics of PsA or the spondyloarthritis group of disorders. It is not uncommon that the diagnosis of PsA is often missed in primary care physicians’ and dermatologists’ offices. An obvious reason is that rather than presenting with florid, active polyarthritis, a number of patients with PsA present with limited disease, such as inflammatory spinal pain, tendinitis, enthesitis or dactylitis.
<strong><em>1. Dactylitis</em></strong>
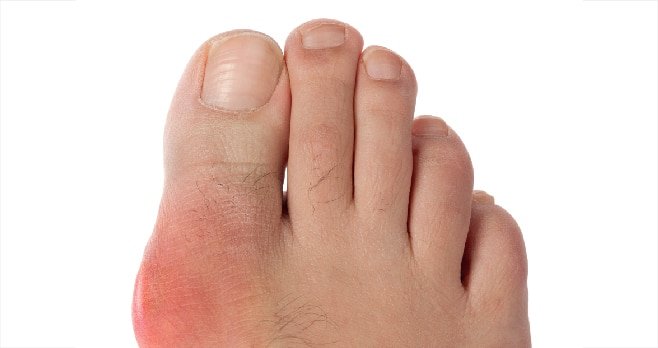
Diffuse inflammation of the tendons, entheses and synovium of nearby joints, occurring simultaneously, lead to the typical ‘sausage’ appearance. It is reassuring that physical examination has shown 100 per cent sensitivity and specificity compared to MRI findings to diagnose tenosynovitis.
Dactylitis is observed in all forms of spondyloarthropathies, with significant specificity in PsA, and this has been included in the classification criteria of PsA, eg, ClASsification of Psoriatic ARthritis (CASPAR) criteria. Dactylitis can be present in up to 48 per cent of patients with PsA, where this can be the first presentation of PsA, and for some time can remain the sole manifestation of this disease. This usually involves toes more than fingers in an asymmetrical distribution and leads to more severe radiological damage.
<strong><em>2. Peripheral arthritis and spondylitis</em></strong>
Although PsA can affect any joint in the body, it typically affects large joints of the lower extremities, distal joints of the fingers and toes, as well as cervical spine and sacroiliac joints. The original diagnostic criteria of Moll and Wright describe five clinical patterns of PsA, which can evolve from one to another:
Asymmetrical, monoarticular and oligoarticular arthritis;
Symmetrical polyarticular arthritis;
Distal interphalangeal joint involvement;
Arthritis mutilans; and
Axial or spondylitis type.
The original studies by Moll and Wright described asymmetrical oligoarthritis as the most frequent clinical pattern of PsA; however, CASPAR database analysis does not support this statement, and concludes that the symmetric polyarticular pattern is the most common presentation.
PsA is characterised by involvement of both the appendicular and axial skeleton. A number of studies have suggested that there are clinical, radiologic and genetic differences between AxPsA (axial PsA) and AS, suggesting that these are distinct entities. Similarly, recent studies examining typical AS-associated genetic risks in AxPsA have largely been negative, further supporting the theory that spinal involvement in PsA is genetically different from that seen in AS.
The spondylitis symptoms typically include pain and stiffness in the areas of the lower back, neck, ribs, hips and thighs. ASAS (Assessment of SpondyloArthritis international Society) inflammatory back pain criteria can be helpful to identify such patients and include: Age at the onset of back pain <40 years; insidious onset; improvement with exercise; no improvement with rest; and nocturnal pain. Inflammatory back pain is present if any four out of these five features are present.
It is quite common that clinical evidence of spondylitis and/or SI occur in conjunction with other subgroups of PsA. For example, patients with peripheral arthritis have quite commonly concomitant inflammatory axial disease, but isolated inflammatory axial disease occurs in less than 5 per cent of PsA patients.
The reported prevalence of axial disease in patients with PsA is quite variable, and has been reported to be as high as up to 78 per cent.
Bilateral sacroiliitis (SI) is more common in PsA than unilateral involvement, but sacroiliitis frequently tends to be asymmetrical. Little is known about the clinical and genetic potential predictors of sacroiliitis in PsA, and we have recently examined clinical and genetic ‘predictors’ of sacroiliitis among patients with PsA. We found that 25 per cent of PsA patients developed SI on long-term follow-up. Severity of skin PsO and the severity of peripheral arthritis had significant association with sacroiliitis. HLA-B*0801 and HLA-B*2705 were genetic predictors for the development of sacroiliitis.
But more importantly, we found that HLA-B*27-positive AxPsA patients have clinical and radiographic features similar to AS, and HLA-B*0801-positive AxPsA patients have radiographic features which are recognised as typical of PsA — asymmetrical and/or unilateral SI.
<strong><em>3. Enthesitis</em></strong>
Entheses are the sites of bony attachments of joint capsules, ligaments and tendons. Inflammatory changes at these sites (enthesopathy) are a prominent manifestation of disease in patients with inflammatory SpA. It is most commonly found at the insertions of the Achilles tendon and the plantar fascia, but may occur in other sites, such as the spine and pelvis, femoral trochanter, humeral epicondyles (commonly known as ‘tennis elbow’ or ‘golfer’s elbow’), tibial tuberosity, patella and olecranon. To examine an entheseal site, sufficient pressure is exerted to blanch the fingernail of the examiner (approximately 4kg). The Leeds enthesitis index is a simple scoring system, which is commonly used for the assessments of the entheses. The entheseal sites included in the Leeds Enthesitis index are: Bilaterally; the lateral epicondyle of the humerus at the common extensor origin; the medial condyle of the femur just superior to the joint line at the origin of the medial collateral ligament; and the posterior prominence of the calcaneum at the insertion of the Achilles tendon. The soft-tissue components of an enthesis are traditionally evaluated by clinical examination based on the presence of tenderness and/or swelling, while x-rays have been used to assess associated bony changes. Enthesitis may be recognised radiographically as spurs and may also be identified using ultrasound scan.
MRI scan reveals bone marrow oedema adjacent to the entheseal insertion sites representing a synovio-entheseal inflammatory complex at the very early stage of PsA, which supports the hypothesis that entheseal inflammation can be a prime or initial target in PsA disease pathogenesis, at least in a proportion of patients. For each entheseal site, an assessment of the adjacent joint in terms of tenderness and soft-tissue swelling should be made in order to distinguish the swelling and tenderness separately at the joint and the juxta-articular entheses.
<h3><strong>Diagnosis</strong></h3>
Currently, there is no single diagnostic laboratory test for PsA. A thorough physical exam, including x-rays and individual medical history, as well as blood work, including a negative test for rheumatoid factor, is helpful in making a diagnosis. Positive serology for anti-cyclic citrullinated peptide (CCP) antibodies, though more prevalent in RA, may be found in 10-to-15 per cent of PsA patients. Acute phase reactants in PsA are frequently normal or minimally elevated, contributing little to diagnosis, and at times can unfortunately lead to a delayed referral. We have recently examined the long-term associations of raised inflammatory markers among patients with PsA, and results were presented at the recent European League Against Rheumatism (EULAR) 2018 annual meeting.
We concluded that since PsA is a heterogeneous disease with <50 per cent of patients developing radiographic damage, raised CRP or ESR can help stratify patients with severe PsA phenotype, not only as regards radiographic damage and more resistant disease to DMARDs and TNF inhibitors, but also having a higher number of significant comorbidities. Many classification criteria of PsA have been proposed, but CASPAR criteria are now the most commonly used and internationally-agreed criteria, and also have the potential to be used for diagnostic purposes (Table 1).
<h3><strong>Comorbidities</strong></h3>
There is considerable evidence to support the assertion that PsA is actually a multi-system disease. In addition to the characteristic extra-articular features, such as uveitis and inflammatory bowel disease, patients with PsA may also suffer from conditions that are related to the consequences of the disease or its treatment. Such co-existing diseases are referred to as comorbidities. Examples of comorbidities in PsA are hypertension, hypercholesterolaemia, diabetes mellitus, obesity, depression and malignancy. The presence of both extra-articular manifestations and comorbidities may have consequences for the treatment, prognosis and outcome of the disease, which frequently go unrecognised or under-treated.
It has become increasingly recognised that the burden of inflammation dictates the presence of such comorbidities. There are a number of studies from our group to support this notion. For example, firstly, we have shown in an in-depth analysis of a long-term follow-up cohort that severity of PsA is significantly associated with the presence of metabolic syndrome and insulin resistance. It is well known that insulin resistance causes endothelial cell dysfunction, subsequently leading to atherosclerosis and finally to end-organ damage, with stroke or myocardial infarction. Secondly, in a different cohort of PsA patients, we showed that metabolic syndrome was much more common than in patients attending rheumatology clinics with non-inflammatory musculoskeletal conditions. Thirdly, we have also recently shown that higher coronary artery plaque burden in PsA is independent of metabolic syndrome and associated with underlying PsA disease severity. Fourthly, we have found that comorbidities using the Charlson Comorbidity Index are significantly associated with erosions and number of deformed joints
Furthermore, the studies from other centres have also shown similar findings. For example, increased burden of inflammation over time is associated with the extent of atherosclerotic plaques in patients with PsA. Another study has shown that cumulative inflammatory burden is independently associated with increased arterial stiffness in patients with psoriatic arthritis.
Inflammation in PsA contributes not only to traditional cardiovascular risk factors (higher BMI, hypertension, diabetes, increased waist circumference and insulin resistance), but also likely causes increased thrombotic tendency. In the same study, authors conclude that a shared inflammatory pathway exists between PsA and obesity, hypertension, dyslipidaemia and insulin resistance.
<h3><strong>Management</strong></h3>
The Group for Research and Assessment of Psoriasis and Psoriatic Arthritis (GRAPPA) and EULAR have published recommendations for the treatment of PsA. The EULAR recommendations focused specifically on musculoskeletal PsA, but no management recommendations were made for skin or nail manifestations.
However, GRAPPA assessed both dermatological and musculoskeletal manifestations, along with recommendations for skin and nail disease. Overall, the recommendations address conventional synthetic DMARDs as an initial therapy after failure of NSAIDs and local therapy for active disease. Potential DMARDs included methotrexate, sulphasalazine and leflunomide.
Furthermore, if necessary, it should be followed by a biologic DMARD or a targeted synthetic DMARD (tsDMARD), such as TNF inhibitors, targeting interleukin (IL)-12/23 (ustekinumab), targeting IL-17 pathways, or a phosphodiesterase 4-inhibitor (apremilast).
<strong>References on request</strong>






Leave a Reply
You must be logged in to post a comment.