The severe challenges facing model 3 hospitals were laid bare in a recent HSE report. David Lynch reports
“I think we have a crisis in the model 3 network.”
That was the stark verdict delivered by the Medical Director of HSE National Doctors Training and Planning (NDTP) at the recent launch of the NDTP’s Model 3 Hospitals Report.

Prof Brian Kinirons
Prof Brian Kinirons was addressing attendees at the national medical workforce conference in November, which included the Minister for Health Stephen Donnelly.
The Minister listened as Prof Kinirons outlined the main points of the report. The report concluded that the future of model 3 hospitals was “precariously balanced” due to challenges with recruitment and retention of consultants.
“I believe if we don’t come up with solutions to this crisis, we will have challenges delivering care in the short-term future,” Prof Kinirons warned at the conference.
Amongst its findings the report identified “marked differences” between model 3 and model 4 hospitals. For instance, in model 3 hospitals 24 per cent of consultants were in locum posts; 7 per cent were not on the specialist division of the Medical Council register; 7 per cent were in non-approved posts; and 33 per cent were over the age of 55. These numbers were significantly higher than in model 4 hospitals.
It noted that while there had been “substantial growth” in the number of consultants employed over recent years, “recruitment and retention of consultants remains a national challenge.”
The new NDTP report makes a number of recommendations, including the need for a “robust” recruitment drive.
“Analysis showed an estimated recruitment need for 1,005 model 3 hospital consultant posts in the next 10 years,” according to the report, which described this target as a “major challenge”.
Speaking to the Medical Independent (MI) at the conference, Prof Kinirons agreed that model 3 hospitals faced “significant and serious” challenges to service delivery due to recruitment difficulties. He told this newspaper that the new consultant contract may somewhat aid recruitment in model 3 hospitals, but the issue is “bigger than the contract”.
“There are some specialties that are more challenged than others and I think there are certain sites more challenged than others,” Prof Kinirons told MI.
“So for example, we know if a model 3 hospital is in reasonable proximity to a model 4 [hospital], recruitment in that model 3 isn’t as difficult… but I think there are a whole series of challenges in relation to model 3 hospitals.”
The report also recommended addressing consultant workload in model 3 hospitals, investing in education and training, improving on-site infrastructure, and reinforcing links with model 4 hospitals.
According to the NDTP report, there are currently 17 model 3 hospitals, divided across five Hospital Groups. In preparation for the report, a survey of NCHDs was conducted. This exposed concerns regarding education and training opportunities. The survey found that only 6 per cent of trainees “express an interest in working in a model 3 hospital”.
“The recruitment challenges, when you are looking at a small model 3 hospital compared to a large teaching hospital, are significant and growing,” Dr Mick Molloy, Consultant in Emergency Medicine in Wexford General Hospital, told MI.

Dr Mick Molloy
Dr Molloy noted that changes in training programmes over the last 20 years saw fewer trainees working in the model 3 network. “They [model 3 hospitals] don’t have the registrars in the hospitals – they don’t [have enough] NCHD posts.”
The former IMO President said that when doctors “are applying for a career post, a consultant position, many have never had the experience of being in the smaller hospital”. As a result, they are more likely to “apply for consultant posts in the large teaching hospitals”.
He said other challenges for model 3 hospitals included more onerous rotas compared to larger city-based hospitals and less “opportunity of postgraduate education”.
The NDTP report identified three specialties that experience the greatest difficulty with consultant recruitment and retention in model 3 hospitals: Radiology; obstetrics and gynaecology; and emergency medicine.
Emergency medicine
Irish Association for Emergency Medicine (IAEM) President Prof Conor Deasy told MI that the Association “welcomed” the increase in consultant numbers in the health sector “across specialties and in emergency medicine specifically”.
However, Prof Deasy, Professor of Emergency Medicine at University College Cork and Clinical Director of Emergency and Acute Care at Cork University Hospital, noted that doctors working in the model 3 sector can face particular challenges.

Prof Conor Deasy
“Clearly people will be wary of taking up consultant posts where they feel isolated, exposed or unsupported,” Prof Deasy said. “Similarly, in the current environment, where there are ample consultant in emergency medicine job opportunities, consultants will opt to work in hospitals where they know the support services are present in radiology, critical care, surgery, medicine, etc.” He said that emergency medicine consultants would be attracted to hospitals where there was a “one team” approach “supported” by the executive management of the hospital and Hospital Group.
But there are also aspects of the working life in the model 3 sector that can be a potential attraction to consultants, he added.
“Often consultants will have a particular connection with the area in which they seek to work and live. A model 3 environment that is smaller, where everyone knows each other and works effectively in a patient-focused manner in support of their community, is very attractive.”
Echoing some of the findings of the NDTP report, Prof Deasy said that “sustainable rotas are vital to avoiding burnout”. He noted that such rotas had traditionally been difficult for model 3 hospitals to achieve. However, he recognised that this had “improved in emergency medicine”.
I believe if we don’t come up with solutions to this crisis, we will have challenges delivering care in the short-term future
“Model 3 hospitals that support trainees on training programmes in emergency medicine also make for a significantly better, more rewarding and resilient working environment,” said the IAEM President.
Radiology
The NDTP report found that radiology trainees do not rotate to model 3 hospitals and that “radiology services are being outsourced to the private sector” in a number of sites.
In this regard, its recommendations included a call to extend radiology training rotations to model 3 hospitals. This extension is to be performed in conjunction with the Faculty of Radiologists. The report also recommended that individual hospitals need to “invest in growing their radiology capacity as the long-term sustainable solution for scheduled and unscheduled care”.
Dr Molloy said radiology infrastructure and workforce were particularly important to model 3 hospitals.
“It has a detrimental effect on recruitment to every service [in model 3 hospitals] if you don’t have a well-resourced radiology department,” he said.
He explained there is a “trend in recent years towards regionalisation of cancer services, and orthopaedic services, and others, and that’s all good from the patient perspective”. But he said this workload had put significant pressure on access to scanning facilities in the model 3 sector.
Dr Molloy added the smaller hospitals are “not fully resourced to deal” with the workload and are working with a “much smaller pool of radiologists and radiographers” compared to model 4 and other hospitals.
In his own emergency medicine role, he said it can be difficult to get access to scans. “Model 3 hospitals… will have a single scan, but there really should be two or three CT scanners,” he said.
He said this under-resourced situation in radiology, and other departments, was a barrier to consultant recruitment to smaller hospitals.
Positives
However, Dr Molloy also identified aspects of model 3 hospital work that can prove attractive to consultants.
“The collegiality, the fact that you are small helps that,” he said. “The fact that you might only have to drive minutes to work, rather than an hour or an hour and a half across the city.”
He also noted “the ability to purchase a house”, “the ability for your kids to get into schools without having significant problems… those are all very attractive.”
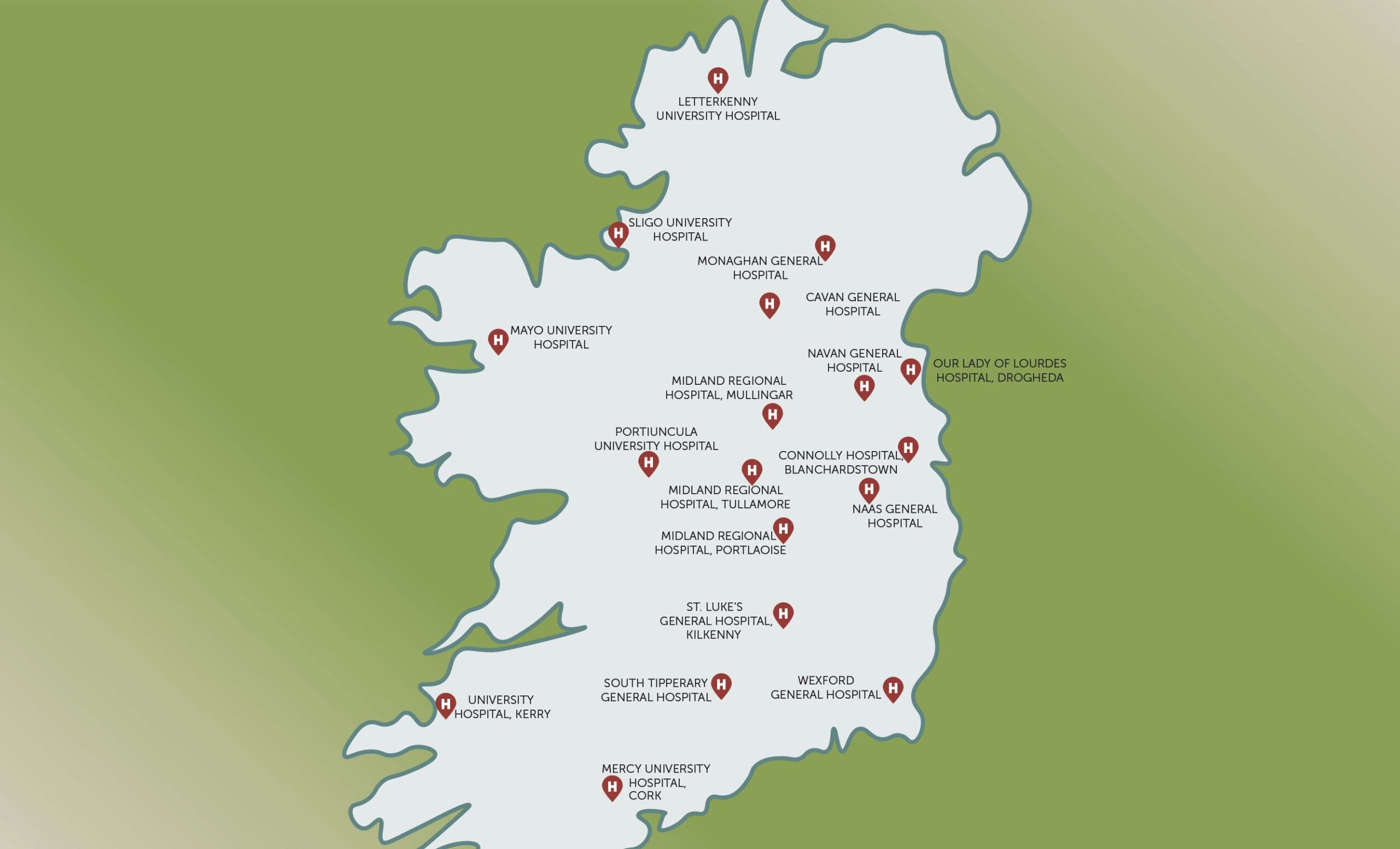
“And to be honest, if you look around the map of the country, the model 3 hospitals are set up in some of the most beautiful areas of Ireland.”
He said these aspects of the “rural lifestyle” may appeal to consultants, particularly those living and working abroad.
“If I had free rein on this, I would be looking around the world at people who are maybe five or 10 years out from retirement in their own country and then ask them, ‘would you like a new challenge?’”
He said the recruitment of experienced consultants was important. With the current and future planned expansion of numbers, it was preferable to not just have “1,000 new consultants who are all 35 years of age”.
“Because in 25 years we will never be able to replace that same number of people again – we need a phased, managed increase.”
Leadership
The leadership of the HSE has said it is taking the model 3 hospital network seriously.

Dr Colm Henry
Addressing the NDTP conference, the HSE Chief Clinical Officer Dr Colm Henry described the new report as a “call to action to invest in model 3 hospitals”.
He told conference attendees about recent demographic research from the UK that showed older people are moving from cities into the rural peripheries in increasing numbers. “There is no reason why we should not expect the same [trend in Ireland],” said Dr Henry. “Hence the model 3 hospitals are important.”
Speaking to MI, Dr Henry said he believed the new consultant contract would support the recruitment of hospital doctors. He said the “reception we hear from newly appointed consultants is that they’re very enthusiastic about it….Enthusiastic not just about the terms and conditions, but the degree of flexibility it gives them.”
Speaking at the same conference, HSE CEO Mr Bernard Gloster told delegates that the model 3 hospitals were a “wonderful concept” and an important part of the planned regionalisation of healthcare. “But if we don’t mind it [model 3 hospitals] and if we don’t think about it now… we will lose its benefit, because we will not be able to sustain the medical workforce in it.”
Important role
Despite the HSE’s stated intentions to sufficiently support model 3 hospitals into the future, Dr Molloy voiced some scepticism. He added, however, that the health service cannot deny the important role they play.
Referencing the fire at Wexford General Hospital last March, Dr Molloy said the incident highlighted the significance of model 3 sites.
“Overnight you had one small hospital taken off the block of the admission processes in the south-east. The rest of the hospitals in the south-east were under significant pressure to try and cope and the impact was felt even as far north as St Vincent’s [University Hospital, Dublin],” he said. “There is just very little slack in the health system at the moment. You can’t afford to take any single hospital out and not suffer significant consequences in the others. That’s the case no matter how small it is.”
Dr Molloy said he believes the incident has helped the HSE to recognise the value of model 3 hospitals “as they have seen the future when just one hospital was taken out”.
However, he said that “you really have to build up the model 3 hospitals” in terms of capacity and resources. Dr Molloy added that “elective-only” hospitals would help the acute sector and he was critical of the slow pace of HSE plans to build three such hospitals in Dublin, Cork, and Galway.
Origins
Writing in the foreword to the NDTP report, Mr Paddy Kenny, RCSI Council Member and Joint Clinical Lead for the National Clinical Programme in Trauma and Orthopaedic Surgery, noted that the report had its origins in RCSI research from 2014. The research was published in 2017 in the Irish Journal of Medical Science.
“It showed an impending surgical workforce crisis in model 3 hospitals, which deliver about 50 per cent of general surgical activity nationally,” wrote Mr Kenny. He outlined that he had approached Prof Kinirons “who felt the issues would be replicated in other specialties”.
“The data gathered and validated by the NDTP has corroborated this prediction,” wrote Mr Kenny.
“As co-sponsors of the project, RCSI warmly welcomes this report which has used the latest data and covered all consultants in model 3 hospitals to reach strong recommendations that address the key issues. It is now incumbent on us all to work towards implementation in the short- and medium-term.”
‘More control over recruitment’ among recommendations
The HSE National Doctors Training and Planning (NDTP) Model 3 Hospitals Report recommends a number of actions, including a specific consultant recruitment campaign. On the high levels of consultant workload in model 3 hospitals, the report recommends that sites should “explore the possibility of Hospital Group/health region rotas or hospital clusters in a defined area if possible”.
In the face of concerns over the length of time taken to fill consultant posts in model 3 hospitals, the report states that statutory hospitals should be given “more control of recruitment within their Hospital Group or health region”.
Model 3 hospitals should “promote and establish” flexible working opportunities to address lifestyle factors and make posts more attractive to all applicants, while hospitals should invest in growing their radiology capacity.
NDTP Medical Director Prof Brian Kinirons told the NDTP’s workforce conference in November that three specific model 3 sites would be selected on the basis of “need and challenge” to pilot these recommendations. Local implementation teams will be established, which will then report back on progress.
Looking broadly at the NDTP report’s recommendations, Consultant in Emergency Medicine Dr Mick Molloy said “you need to try everything”.
“Those things are great ideas, but I’m not sure on their own that any single one of them would be the thing [to address recruitment challenges].”
He believed the health system needed to “manage” emigration better. Dr Molloy proposed a scheme that would see the HSE approach doctors in the “second last year or the third last year” of their senior registrar programme and offer to fund the salary of the doctor to work in a health system abroad for a couple of years, as long as they committed to return to Ireland to work in a model 3 hospital for a set number of years.
He also voiced concerns that the expansion of consultant numbers across all hospitals may make it more difficult for model 3 hospitals to recruit in the coming period.
With the six new health regions due to commence next month, Prof Kinirons told the conference that “it is very clear for our health regions we need a sustainable, robust, model 3 network”.
“What is of concern to me is that about a quarter of the entire workforce in the model 3 network are on a non-permanent contract,” Prof Kinirons told the conference, “and if that does not ring alarm bells, I do not know what will.”
The “age profile” of consultants in the model 3 network was “more senior” than their model 4 network colleagues. One-third of the consultant workforce in model 3 hospitals was 55 years old or greater.
Prof Kinirons added that “it will come as no surprise to you that a constant recurring theme was the fact that many sites felt that the consultant recruitment process was not fit-for-purpose”. Consultants reported that the process was “complex”, “too slow”, and not “responsive”.
He said that recruitment processes at a more local level led to more positive experiences for consultants.
Infrastructure deficiencies were also raised by model 3 hospital consultants.
“Not just physical infrastructure, but digital infrastructure,” said Prof Kinirons.
He outlined challenges for trainees in model 3 hospitals. “While there were sites that had excellent support infrastructure for education and training, there were many sites where that support was either inadequate or absent.”
Specialist division and model 3 hospitals
In late November 2023, there were 103 consultants employed by the HSE across the health system who were not on the Medical Council’s specialist register, according to figures provided to the Medical Independent (MI).
The recent HSE National Doctors Training and Planning (NDTP) report into model 3 hospitals highlighted the relatively high number of doctors not on the specialist register employed in these hospitals.
The report found that 7 per cent of model 3 hospital consultants were not on the specialist register compared to just 1 per cent in model 4 hospitals.
Speaking in November, Medical Director of NDTP Prof Brian Kinirons said it was “a source of concern to see that up to 7 per cent of the workforce are on the general register, rather than the specialist register”.
“Again, that represents challenges,” he said.
Speaking to MI in October, the IHCA President Prof Robert Landers said employing doctors in consultant posts, without specialist registration, was a “major concern”.
“Consultants should be on the specialist register of the Irish Medical Council [which] is the regulatory body for maintaining standards in Irish medicine,” he commented.












Leave a Reply
You must be logged in to post a comment.