Clinicians are urging the establishment of a national clinical programme for haemoglobinopathies
against the backdrop of a groundbreaking UK report on care failures. Catherine Reilly reports
Some patients with sickle cell disease (SCD) are at increased risk of life-changing complications as they cannot access chronic blood transfusion programmes at St James’s Hospital in Dublin.
St James’s provides the only specialist service in Ireland for adults with this serious inherited blood disorder. However, it has insufficient ambulatory care and laboratory capacity to provide transfusion programmes to all patients requiring them, the Medical Independent (MI) understands.
SCD, the commonest haemoglobinopathy, is most prevalent in people of African or Caribbean background. Chronic transfusion is an essential treatment for many patients. The St James’s service highlighted “urgent” requirements, including sufficient day-ward capacity to transfuse patients, in business cases submitted to the HSE in 2021 and 2022, according to documents obtained under Freedom of Information law.
Consultant Haematologist Dr Emma Tuohy told MI that 12 of her patients are on a waiting list to commence blood transfusion programmes (one patient with thalassaemia; 11 with SCD).
An ambulatory care unit and recruitment of additional medical scientists for the transfusion laboratory are urgently required.
“There are patients who could develop life-changing complications if I cannot transfuse them,” said Dr Tuohy, who leads the haemoglobinopathy/red cell disorders service at St James’s.
There are just two treatment bays designated to the haemoglobinopathy service, which has approximately 280 patients (255 have SCD). Sixty-four of the patients are receiving chronic transfusion programmes (56 patients have SCD, the remainder have thalassaemia/rare red cell disorders).
Approximately 90 young adults aged 18 and over (including around 40 on transfusion programmes) are attending Children’s Health Ireland (CHI) at Crumlin, which has around 380 patients with haemoglobinopathies. The high-risk transition stage is managed carefully between the paediatric and adult services. They prepare patients for an anticipated move to the adult service at 18/19 years of age or after the first year of college. However, St James’s does not currently have capacity to take the patients reaching this age range.
CHI Crumlin and St James’s are the only national comprehensive services with expertise in management of haemoglobinopathies. They are EU-recognised expert centres for haemoglobin/red cell disorders as part of the Eurobloodnet European Reference Network in Rare Haematological Diseases. However, they are not designated as national referral centres with associated resourcing and a national model of care.
On 31 March 2022, in the Dáil, Minister for Health Stephen Donnelly acknowledged “real challenges” in the capacity of St James’s to receive SCD patients from Crumlin. He also maintained it was a HSE priority to “further advance the non-malignant haematology service at CHI Crumlin”.
He was responding to Deputy Duncan Smith (Labour), who had met with the CEO of Sickle Cell and Thalassemia Ireland Ms Lora Ruth Wogu, and board member Ms Ijeoma Nwabuezi.
“One of their key concerns is how under pressure the St James’s service is. The service at St James’s Hospital, and the clinicians, are fantastic but they are under pressure,” Deputy Smith told the Minister.
St James’s received approval for additional staffing from the HSE. A HSE spokesperson said €1.2 million non-pay funding was allocated to St James’s in August 2022 to provide the “necessary transfusion services for patients awaiting transfer to the service from CHI”.
However, records obtained by MI indicated an historical under-funding of these costs, which were continuing to grow with the numbers requiring transfusion programmes. The lack of an ambulatory care unit remains a critical deficit (the 2022 business case stated a full review of capital costs would be conducted separately).
Increasing numbers
St James’s is also receiving 20 to 30 new haemoglobinopathy referrals per year – this number is rising in line with migration patterns. Currently, the service cannot accept all referrals due to the capacity constraints. Dr Tuohy provides advice on patient management to haematologists at other hospitals. The St James’s team can also take over the management of patients in instances where they are acutely unwell.
A dramatic rise in adult patients was forecasted by clinicians due to the age profile of a significant cohort at Crumlin. In 2014, 32 patients attended St James’s, and in 2021 this had risen to over 220.
In March 2021, St James’s CEO Prof Mary Day wrote to the then HSE Director of Acute Operations Mr Liam Woods conveying the “urgent requirement for a model of care” for haemoglobinopathies.
She stated the main requirements were designation as a national adult centre; a national patient database in conjunction with CHI; increased staffing and funding; a designated ambulatory care unit; protected inpatient beds; and development of an appropriately accredited laboratory.
The business case, dated December 2020, stated the service did “not currently have the necessary day-ward capacity to transfuse all our patients and meet the constant increasing demands. This will have a significant impact on emergency department admissions in the future, as well as an additional requirement for inpatient beds.” Fourteen patients were waiting to transfer from the paediatric service and all were on transfusion programmes.
According to an updated business case, dated March 2022, 58 patients were
awaiting imminent transfer and 41 were on transfusion programmes (24 were aged 19-22 years and needed to “urgently” transfer to the adult service).
The delayed transfer incurred “a significant clinical risk to these patients, as they are too old to access appropriate care”. The situation was also concerning from a child protection perspective.
The business case referred to the HSE’s Model of Care for Transition from Paediatric to Adult Healthcare Providers in Rare Diseases (2018), which highlights the serious risks to patients of a poorly planned transition.
In late 2020 the service received some additional space (ie, the two treatment bays) through investment by St James’s, but it was insufficient, according to the business case. It noted that a designated ambulatory care unit would also facilitate the triage and outpatient care of some patients who otherwise would have presented to the emergency department and been admitted.
Haemoglobinopathies
Haemoglobinopathies (SCD and thalassaemia) are autosomal recessive inherited conditions affecting the haemoglobin component of blood. SCD is probably the most common severe inherited disease in the world, but a low priority on the agenda of governments, and the haematology and global health communities, according to The Lancet Haematology Commission on SCD (2023).
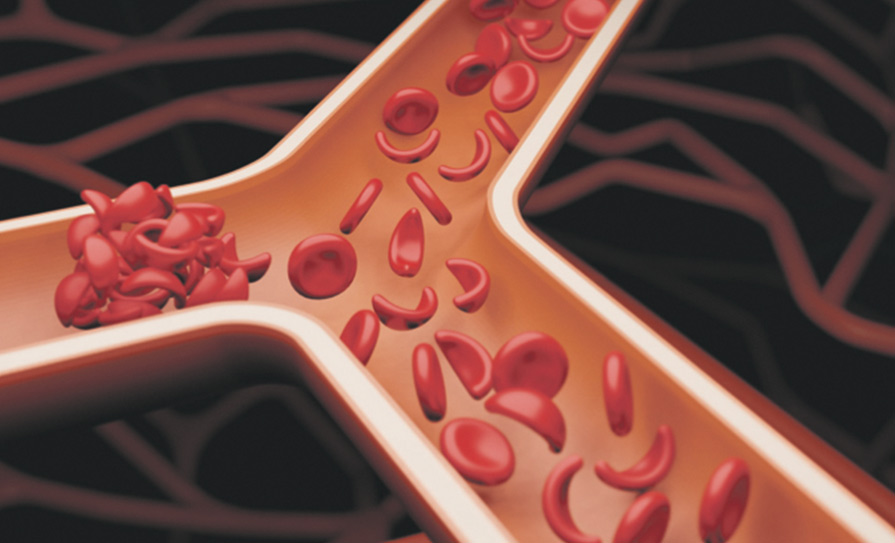
SCD is characterised by abnormal, rigid, ‘sickle’ shaped haemoglobin. These sickled red blood cells restrict the flow in blood vessels and limit delivery of oxygen to the body’s tissues.
The condition has three major features – hyposplenism; anaemia; and vaso-occlusion. Hyposplenism can lead to severe infection and death. Anaemia causes fatigue and has been linked to brain injury and long-term lung damage. Vaso-occlusion can cause severe pain, tissue death, and chronic damage. Tissue damage can lead to stroke, blindness, respiratory failure, bone disease, and renal failure.
In higher income countries, significant reductions in childhood mortality have been achieved. This has largely involved new-born screening, anti-pneumococcal penicillin prophylaxis and vaccination, transcranial Doppler ultrasound, early introduction of disease-modifying treatment, co-ordinated follow-up, and parental education.
The main disease-modifying interventions are hydroxycarbamide (hydroxyurea) and chronic blood transfusion programmes (top-up transfusion and red cell exchange). Practical steps to reduce the risk of a crisis include staying well-hydrated, avoiding extreme temperatures, avoiding very strenuous physical activity, and minimising stress.
However, patients with SCD are intermittently unwell. Vaso-occlusive episodes and crises can occur unpredictably and vary in duration and severity. Patients with complicated crises can deteriorate quickly.
While the course of illness can differ, evidence of end-organ damage manifests as patients age, contributing to increased morbidity and early mortality. The condition can have significant implications for patients’ mental health, employment status, and overall quality-of-life.
‘No-one’s listening’
In November 2021, a UK all-party parliamentary group published No one’s listening: An inquiry into the avoidable deaths and failures of care for sickle cell patients in secondary care. The report found that the care in specialist haemoglobinopathy services was “generally felt to be of a good standard”. However, this was not the case in general wards and emergency departments (EDs).
There was a “routine failure” to comply with national care standards or NICE pain relief standards when patients attended EDs; a lack of effective joined-up care including communication failings between different departments within the same hospitals; patients regularly had to educate healthcare professionals about the basics of their condition at times of significant distress; and there was inadequate investment in sickle cell care and research.
Many of those who provided evidence highlighted the role of racism in the negative attitudes towards patients. Shortfalls in care had led to avoidable deaths and near misses, according to the report.
No-one’s listening was referenced in the 2022 St James’s business case, which said Ireland could learn from evidence of shortcomings in other jurisdictions.
The Haematology Association of Ireland also wrote to Minister Donnelly on foot of the UK report, urging the appropriate resourcing of specialist services, and establishment of a national clinical programme.
Paediatric service
Writing in the Irish Journal of Medical Science in 2001, Consultant Paediatric Haematologist Prof Corrina McMahon highlighted the need for “a comprehensive care approach” for an increasing cohort of SCD patients. In the mid-to-late 1990s, there were less than 20 people known to have SCD in Ireland. In the early 2000s, as the country became more multi-ethnic, there was a rapid rise in presentations.
Since that time, Prof McMahon has led the development of the paediatric service – advocating for comprehensive care at various fora and developing linkages with paediatricians nationally.
Speaking to MI last month, Prof McMahon emphasised that SCD could inflict serious morbidity, as well as the mortality risk.
“When sickle goes bad, it is devastating,” she said.
The CHI service provides comprehensive care and management strategies, in conjunction with other departments. But it has never received specific funding for its national role.
Prof McMahon said peer reviews have delivered positive findings on quality of care, but have flagged under-staffing.
Two consultants, including Prof McMahon, manage haemoglobinopathies and other red cell disorders. They also receive consults and requests for clinical advice from around the country and provide clinical leadership for the general haematology and blood transfusion laboratories, among other duties.
The service had only two nurses for many years, although support to recruit two more nurses has been received through funding for benign haematology. The wider multidisciplinary team is a shared resource with other busy services.
Two more consultants specialising in haemoglobinopathies, and a quality manager, are among the additional posts required, stated Prof McMahon. She further noted a need for consultant resources specifically for care during the transition process (in the paediatric and adult services). Some trainees rotating to the paediatric service have expressed an interest in specialisation, but Prof McMahon said new consultant posts are required to benefit from this engagement.
Asked about adult patients stuck in the paediatric service, Prof McMahon confirmed this creates a myriad of issues. Care in a children’s hospital is no longer appropriate, and it impacts patients developing their relationship with the adult service. It also has repercussions for CHI’s capacity.
“They do ask every now and again, when are we going? So they can prepare themselves. And we have to say, we are not entirely sure when you are going.”
Newborns
In recent years there have been 10-14 referrals per annum, including newborns. However, this year the service has already received 10 referrals.
An unfunded targeted newborn screening programme (based on high-risk ethnicities) was established by Crumlin with maternity units in the mid-2000s. This followed the deaths of two babies who had not been diagnosed.
However, due to certain impositions under GDPR, these arrangements have become less robust. Prof McMahon said there had been a decline in samples received.
In 2018, SCD clinical experts from across Europe (including Prof McMahon) published a consensus statement in the British Journal of Haematology recommending universal newborn screening for SCD in their countries. To date, SCD has not been added to the National Newborn Bloodspot Screening Programme (NNBSP), which screens for nine conditions compared with the European average of 18.
A Department of Health spokesperson said SCD is on the work programme of the national screening advisory committee in terms of further consideration.
When sickle goes bad, it is devastating
HSCT
Another vital requirement is access to haematopoietic stem cell transplantation (HSCT). The national paediatric HSCT unit is based at Crumlin, but SCD is not among the conditions provided for.
While gene therapy offers promise, HSCT is the only established curative treatment for clinically eligible patients, who require a matched donor (usually a sibling).
Currently, CHI is aiming to facilitate access at St Mary’s Hospital/Imperial Healthcare NHS Trust in London.
There are significant practical and financial impediments to patients accessing the procedure via the Treatment Abroad Scheme. In 2023, a health technology assessment by HIQA recommended ‘repatriation’ of paediatric HSCT for certain rare inherited disorders, including haemoglobinopathies.
Prof McMahon and Dr Tuohy believe HSCT should be resourced in Ireland for eligible patients. Access to new medications and increased clinical trial activity are other goals.
In the ‘Celtic Tiger’ era, the State had ample finances to resource the CHI service. MI asked Prof McMahon if the lack of State investment was due to the patients’ ethnic background. She said her impression was of political disinterest as many families had no national voting rights at the time. “Other people were shouting louder, and people with votes were shouting louder,” she stated. She also noted a general lack of strategic planning by health authorities which has long impacted the health service.
Prof McMahon said there is concern among staff for the wellbeing of patients amid the recent rise of far-right sentiments in parts of Irish society.
Looking ahead, Prof McMahon strongly believes a national clinical programme for haemoglobinopathies is required. She said this would promote engagement on SCD across healthcare and the development of a nationally agreed model of care, as has occurred in other disease areas. She said the findings from the UK report, No-one’s listening, must be heeded.
Dr Tuohy at St James’s echoed these remarks. “We need a national framework so we can manage these patients in a hub and spoke model,” she said.
A national clinical programme would also support the best practice management of acute presentations in EDs nationally.
Dr Tuohy said international research has established that many patients do not present to healthcare due to fear of how they will be treated and lack of knowledge of SCD management, including appropriate analgesia.
Dr Tuohy said these issues have also been reported by patients in Ireland.
By the end of 2030, it is projected that 540 patients with SCD will need to attend the adult service.
There is also increasing complexity of care, including management of women in pregnancy, who are jointly managed by St James’s and the Coombe Women and Infants University Hospital, Dublin. The standard of care was described as “exemplary” following review at a clinical forum of the Hospital Group. Seven babies have been born to mothers with SCD at St James’s since 2014.
Dr Tuohy will be joined by another consultant in the coming months. She hopes that trainees on the haematology specialist training scheme will have the opportunity to rotate through the adult red cell service, which will help support future subspecialisation and enhance the experience of all haematologists in managing haemoglobinopathies in adult services.
The HSE has informed MI it does not currently consider a clinical programme necessary to advance planning and delivery of haemoglobinopathy services, but “this will be kept under review”.
The spokesperson said the HSE is “committed to responding to the increasing need for services for children and adults living with haemoglobinopathies”.
Meanwhile, the Irish Blood Transfusion Service (IBTS) is considering a targeted advertising campaign on blood donation aimed at communities of African background, among other initiatives.
To prevent alloimmunisation and ensure availability of appropriately matched transfusions for SCD patients, more people of African background are needed in the donor pool. This is also of critical importance to reduce the ongoing pressure on O negative blood stocks.
The IBTS introduced malaria antibody testing in May 2023, which has enabled it to begin running specific “African heritage recruitment drives”
‘That five minutes could change the child’s life’


Nigerian-born Ms Esther Onolememen is the founder of Sickle Cell Society Ireland, a parent- and patient-led support group for people impacted by SCD in Ireland. She also sits on the board of the Irish Patients Association as the Director of Diversity and Inclusion.
The Society seeks to empower people with SCD, and their families and friends, to become agents of change. It uses fashion shows and sports events to generate greater awareness of the condition. It has held early patient contact modules for medical students at the RCSI and University College Dublin.
Its foundations were laid in 2006 during Ms Onolememen’s master’s thesis at Trinity College Dublin, which examined the experiences of African parents of children with SCD in Ireland. The stigma and lack of support felt by affected communities were among the prominent issues raised in her research.
However, Ms Onolememen’s interest in this area is not merely academic. Two of her children, Debbie, and the late Reme, were born with the condition.
Reme was 22-years-old when she died at St James’s Hospital on 1 March 2023. The family said Reme spent around 24 hours in the ED awaiting admission. She was in her final year of studying youth and community development.
The passing of Reme is very raw for the family.
To give voice to her feelings, Debbie – a final-year medical student – wrote a letter expressing the urgent need for improvements in the ED. With the assistance of the Irish Patients Association, the letter was sent to HSE Chief Clinical Officer Dr Colm Henry and National Clinical Lead for Emergency Medicine Dr Gerry McCarthy.
Speaking to the Medical Independent, Debbie described her letter as a “call to action” for healthcare services to ensure timely and appropriate identification and management of people with SCD.
“I spoke about that, and how patients usually present with acute crises and can deteriorate really quickly if not taken care of promptly,” she said.
Esther Onolememen said they have been informed of improvements in the management of SCD patients at St James’s ED following Reme’s death.
The family want to see more awareness of the condition across healthcare settings nationally.
“Every five minutes for any child with sickle cell in crisis matters a lot. That five minutes could change the child’s life,” stated Esther.
In the aftermath of Reme’s passing, when other parents visited to offer their condolences, she heard stories about ED waiting times. “A lot of people were angry about how long they have to wait.
I wasn’t in that headspace [to take in the precise details] but could hear people talk on the side about different experiences, about the adult ED services, which is quite disheartening.”
As a social worker employed in the public health service, Esther said she can appreciate the nature of doctors’ rotations to different services and their unfamiliarity with a patient’s history.
However, she said with the appropriate awareness and information, EDs “will definitely do better”.
Over time, she noted improvements in the management of acute presentations of SCD at the Crumlin ED, and she said this must be replicated nationally. It is understood the Irish Association for Emergency Medicine is finalising a clinical guideline on SCD.
The Society recently published a pilot study on the experiences of people with SCD in Ireland. The project was funded by the Department of Children, Equality, Disability, Inclusion and Youth under a funding call for the International Decade for People of African Descent.
In-depth semi-structured interviews were conducted with six participants. Thematic analysis revealed inconsistent and often inadequate healthcare access; significant financial burdens; and a lack of awareness among both healthcare providers and the public.
Participants highlighted the substantial psychological and social impacts of SCD, including stigma and mental health struggles.
The study underscored the urgent need for policy interventions to improve healthcare accessibility, financial support, and public awareness.
“We hope that in the future we can do more,” commented Esther, noting the need for greater State support for its endeavours.
Reflecting on her journey, she said it breaks her heart that her children must advocate for the same things she has advocated for.
“Debbie was born in Ireland. Things I have advocated for since she was born, she still has to advocate for it to date…. It is really, really heartbreaking, I am almost being put to tears as I am saying this. What I have had to advocate for, over 22 years ago, my daughter Reme before she passed, even in hospital, would advocate for herself….
“I am very much aware that some of these challenges are not the fault of the healthcare providers – they work within very tight resource constraints, they work within very tight budgets, within a very tight shortage of staff, shortage of specialty, shortage of almost everything. So, where do we put our pressures on? Sometimes I feel as though our voices are not being heard.”
Today, added Esther, many young people with SCD and sickle cell trait in Ireland are forming serious relationships. She said these young people need access to professional support and counselling to make informed decisions. Esther said she knows of couples who were unaware of the potential for their child to have SCD. “It happens, and they are not ready for it. There are so many scenarios,” she said.
She is critical of language that proposes ‘elimination’ of the condition, and the stigmatisation of those impacted. People with such views need to be properly informed, she said.
“It is like saying Debbie, Reme when she was alive, and everyone else, shouldn’t have been born. If you ask me I would give birth to my daughters a million times over, regardless of their sickle cell. All I am asking is the care is in place to manage their sickle cell. And once that care is in place they can live a healthy life.”
The family have founded the Reme Onolememen Sickle Cell Research Foundation (ROSCRF).
As Debbie noted, research on SCD is “hugely under-represented” in the literature. She said the number of research articles on SCD available through Pubmed is half that of cystic fibrosis, for example.
“And we think that this is one of the reasons as to why there is slower progression as to cures and treatments,” she commented.
Through ROSCRF “we hope to bridge the gap” and ultimately improve the quality of care for people with SCD,
said Debbie.
“Honestly, we know that it is going to take baby steps, for sure.”












Leave a Reply
You must be logged in to post a comment.