The proposed regional division of the health service is the biggest structural change in over a decade. Paul Mulholland examines a Department of Health document, which explains the reasons for the division and the challenges that lie ahead
On 17 July it was announced that the health service would be divided into six regional health bodies. Stakeholders in each of the regional health areas have been invited to contribute to the design of the services for their new regions. Work is also being undertaken to detail the national and regional organisational design, which will be brought back to Government for approval next year. The proposal, which follows on from a recommendation in the Sláintecare Report, is the most significant restructuring of the health service since the creation of the HSE in 2004, even considering the formation of the Hospital Groups a decade later. Following the publication of the Higgins report in 2013, seven Hospital Groups have been created. However, the Groups have not progressed as originally intended. The original plan was for the Groups to become Hospital Trusts, yet legislation to allow this to happen has not been forthcoming. Also, the lack of alignment between the Hospital Groups and Community Healthcare Organisations (CHO) has received criticism.
A public consultation on the process of geographic alignment of CHOs and Hospital Groups was conducted by the Department of Health in April and May 2018. According to the consultation, the majority of organisations and individuals were “strongly in favour of the geographical alignment of CHOs and Hospital Groups”. Potential disadvantages cited included disruption to services and structures. In contrast, the possible advantages were more efficient use of resources; better coordination between different care sectors; and the increased ability to conduct population-based health planning.
An internal Department document obtained by the Medical Independent (MI) sheds further light on these issues. The determination of the optimal geographies to underpin the establishment of regional integreated care organisations was completed by the research and development and health analytics division of the Department in November 2018.
The document noted: “In response to the particular problem of the lack of co-ordination across different levels of care, and with the aim of transforming a collection of fragmented services into a person-centred, balanced, managed continuum many governments have issued policies fostering the introduction of regional integrated healthcare organisations or networks.” Within Ireland, the report acknowledged that the issue of delivering care through regions, based on geographic facts and population size, has been discussed as far back as the Fitzgerald report in 1968.
Although some commentators say the new structure is a return to the old health service, the document does not state the health boards were a consideration in drawing up the new regions.
Evidence
Statistical analysis conducted by the Department show there is “evident variation” in the extent to which the hospitals located in an area treated patients from that area. This ranges from 96 per cent of patients attending hospitals in CHO 3 who live in CHO 3, to 62 per cent of patients attending hospitals in CHO 7 who live in CHO 7.
“The analysis undertaken confirms that highly specialist services are accessed by a national patient base and this will continue as the implementation of geographical alignment will not impose restrictions on patient access to specialist national services,” the report stated.
Proposed geography
According to the document: “Further to the assessment of current alignment on the basis of patient pathways and service usage patterns for community and acute care, a range of further options were developed and evaluated on the basis of the factors, which emerged from the research and policy work.”
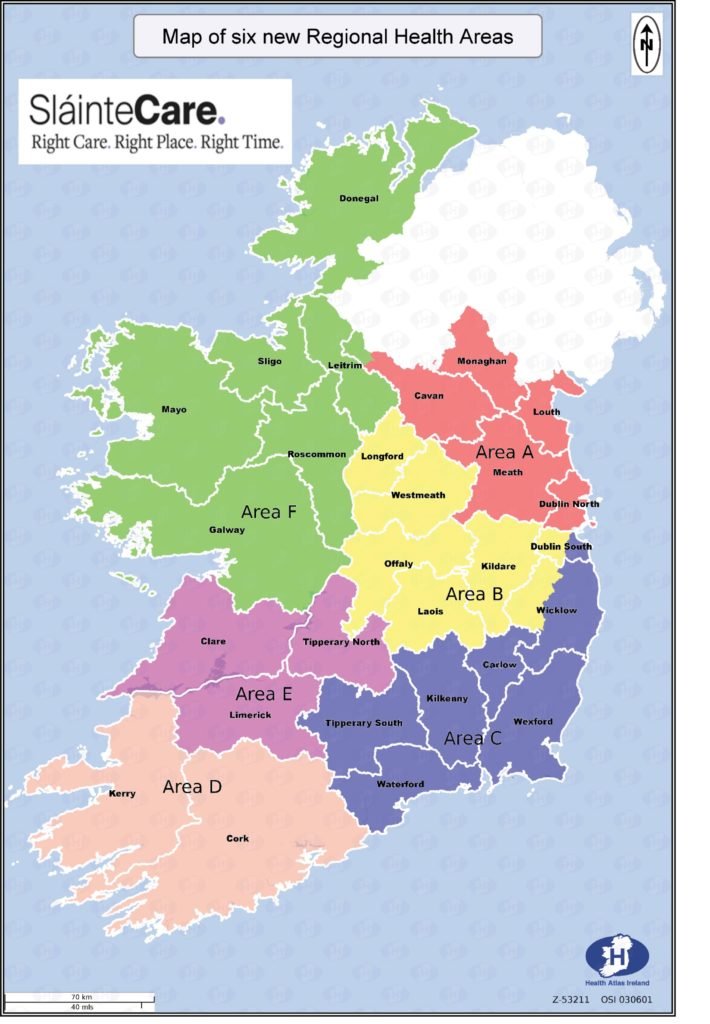
These factors informed the development and assessment of a range of hypothetical structures and geographies intended to improve geographical alignment between hospital and CHOs. Eventually six regions were decided upon (see map). All potential future structures were assessed as to the extent to which they maximised the continuity of current patient flows between community and acute care. According to the document, the proposed six regions registered the highest levels of ‘patient self-containment scores’ of such a regional division.
In calling for geographic alignment and the development of regional integrated care organisations, the Sláintecare Report asked for this to be achieved with “minimal disruption”, particularly with regard to primary care networks.
“The proposed geographies represents the minimum amount of disruption to existing CHOs and HG structures necessary to achieve geographical alignment,” according to the document.
“Any changes to CHOs are proposed on the basis of no disruption of boundries for the underlying LHOs (local health offices).
Also, the report noted that while international reviews show substantial variation in the sizing of health regions, insights from previous policy reviews in Ireland suggest a minimum population size for a health region of approximately 350,000.
“All of the proposed regions exceed the minimum threshold of 350,000 with populations ranging from 385,000 in proposed Area E (mid-west) to regional populations of approximately one million in proposed Area A and C (east-north and south-east.)”
Also, each of proposed regions includes at least one model 4 hospital, one maternity hospital, one national cancer centre and a “comprehensive range of primary and community care services”.
Although the design and details of the management of the new regions was not the scope of the document, the Department also aimed to achieve integration “without an overly complex structure and without too many tiers of management”.
“The regions proposed seek to promote manageability by limiting the span of control to no more than two existing CHOs or to an existing CHO plus two complete local healthcare offices. In terms of manageability for change for hospitals, the six region option (plus national children’s hospital) corresponds in terms of the number of regions with the current number of Hospital Groups.”
The document states that the “feasibility of implementation” is supported in the east of the country by the functional commuting patterns along the national motorway network and in the west by regional identity and established service usage patterns.
“Grouping hospitals by region results in generally improved access times for patients and reduced travel times between hospitals in the groupings.”
However, the document noted that under all the scenarios, including the “optimal geography”, the north west will continue to have access challenges in terms of access to a model 4 hospital.
“This has been alleviated substantially by North-South cooperation, continuation of which will remain vital in the delivery of health services in the north-west and border region.”
It was not deemed critical in the design of geographical areas, that each hospital should only have linkages with academic partners inside their regions.
Disruption
In spite of the attempt to make the transition to the new arrangements as smooth as possible, the document admited that management structures in the acute sector will be disrupted by the proposed regional division.
According to the document, the Ireland East Hospital Group and the South/South West Hospital Group will be most affected by the new arrangements.
“The optimal approach minimises but does not avoid disruption and the entities most disrupted by the achievement of coherent healthcare delivery regions is the current hospital groupings in the acute sector.”
“A changed management challenge arises in particular in Ireland East and South/South West.”
The document stated that the “learning achieved” over recent years in the creation of Hospital Groups and CHOs will be important in the establishment of the regional integrated healthcare organisations.
“On balance, the geographies proposed represent the least change necessary to achieve alignment of health and social care services at regional level.”
When questioned on this issue, a spokesperson for the Department told MI that the level of disruption is low where existing CHOs and Hospital Groups are closely aligned.
“For example new Area E maps exactly to CHO3 and UL (University of Limerick) Hospital Group; Area F maps exactly to the Saolta Hospital Group and fully to CHO2 but not fully to CHO1; Area B maps fully to CHO7 but not fully to CHO8 and closely matches Dublin Midlands HG with the addition of Mullingar hospital,” according to the spokersperson.
“It is acknowledged that there is more disruption in relation to forming Areas A and C due to the existing misalignment of Hospital Groups to CHOs,” according to the spokesperson.
The spokesperson said that any disruption caused “will result in changes to management structures and won’t impact on patients or staff generally”.













Leave a Reply
You must be logged in to post a comment.