<h3><strong>Eczema</strong></h3>
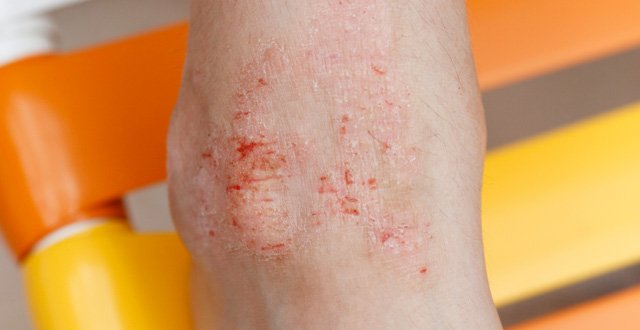
‘Eczema’ is a term often used to describe dry, scaly, itchy skin conditions and is a synonym for atopic dermatitis. Eczema is a chronic, pruritic inflammatory skin disease that occurs most frequently in children, but also affects adults. It is often associated with elevated serum level of immunoglobulin E and a personal or family history of atopy, which describes a group of disorders that includes eczema, asthma and allergic rhinitis.
<h3><strong>Pathophysiology</strong></h3>
Eczematous tissue produces less fats and oils, reducing moisture retention in the skin. As dehydrated surface cells shrink, itching and dryness emerge. Gaps appear between skin cells, allowing irritant substances to penetrate the skin, further triggering an immune response. Inflammation and cracked, weeping and sometimes infected skin result.
Genes and environmental factors are understood to form the basis of eczema. Genetic defects in the filaggrin gene (FLG) involved in epidermal keratin production are thought to cause atopic responses. Additionally, high domestic water calcium carbonate and chlorine levels have been associated with increased risk of eczema in infancy.
People with eczema can have a severely impaired quality of life, with the discomfort of their condition and body image issues preventing engagement in social activities. Itching can be so intense that it prevents sleep, which can impair work and school performances. Children with eczema often ‘grow out’ of their condition by puberty, although they generally will become adults with more sensitive skin than the general population. The more severe a childhood presentation of eczema, the more likely it will persist into adulthood.
<h3><strong>Diagnosis</strong></h3>
The UK’s National Institute for Health and Care Excellence (NICE) defines a positive diagnosis of atopic dermatitis in patients with itching and at least three of the following:
1. A history of involvement of the skin creases/flexures.
2. A personal history of asthma or hay fever (or atopic disease in a first-degree relative of a child aged under four years).
3. Long-term dry skin.
4. Onset at age under two years.
5. Visible flexural eczema (cheeks, forehead or outer aspects of the limbs).
<h3><strong>Non-pharmacological management</strong></h3>
The following are simple measures that can be advised to help improve eczema:
Use cotton clothing and bedding.
Avoid woollen textiles.
Use non-biological washing powder.
Keep nails cut short.
Keep room temperatures cool, as heat may trigger itching.
<h3><strong>Pharmacological management</strong></h3>
Emollients should be used regularly for the moisturisation of eczematous skin. Where emollients do not provide an adequate response, the addition of mild-potency topical corticosteroids are recommended for mild eczema, increased in strength as severity increases. Bandages with emollient may also be used, but occlusion of lesions is not recommended due to the drying effects.
Topical calcineurin inhibitors such as tacrolimus can be introduced for moderate-to-severe eczema in patients who are unresponsive to or intolerant of steroid therapy. Treatment with these agents needs to be monitored closely and is not recommended for continuous use.
In severe eczema, psoralens with UVA (PUVA) phototherapy may be recommended under specialist supervision. Occasionally, systemic therapy with a retinoid or the immunosuppressing therapy cyclosporin is considered.
NICE cautions against the routine use of oral antihistamines in eczema. Where itching is severe, a trial of a non-sedating antihistamine for a month may be reasonable. Age-appropriate sedative antihistamines may aid children if flare-ups are causing sleep deprivation, but these are recommended only for occasional use.
<h3><strong>Psoriasis</strong></h3>
Psoriasis is an inflammatory skin disease that is currently incurable but is amenable to treatment. It is estimated to affect 1.3-to-2.2 per cent of the population in the UK, and affects at least 73,000 people in Ireland. The condition can occur at any age and, although the majority of cases occur before the age of 35 years, it is uncommon in children.
A proportion of patients also have an associated joint disease (psoriatic arthritis), while those with severe disease may be at increased risk of cardiovascular disease, lymphoma and non-melanoma skin cancer. The cause of psoriasis is not known, but inheritance appears to play a part in some individuals. Approximately one-third of patients have a family history and a number of genetic markers have been identified.
Psoriasis normally follows a relapsing and remitting course. Although people with psoriasis are rarely completely clear of diseased skin, there can be long periods when the disease is confined to a small patch on the leg or elbow. They are also likely to experience phases of active disease (flare-ups or exacerbations) and inflamed (red, thickened, scaling) plaques can appear anywhere on the skin.
Psoriasis has a profound impact on the functional, psychological and social dimensions of life and this has important implications for effective management.
The significant reduction in quality of life and psychosocial disability suffered by people with psoriasis underlines the need for prompt, effective treatment and long-term disease control. The relapsing and remitting pattern of the disease imposes a significant burden and means that many patients with psoriasis live with a constant fear that the disease will flare up. Visible lesions (for example, on the hands and scalp) have a greater psychosocial impact than lesions that can be more easily covered up.
<h3><strong>Clinical features</strong></h3>
Plaque psoriasis is the most common clinical form of the condition, accounting for about 90 per cent of patients with the disease. It is also known as <em>psoriasis vulgaris</em> or chronic (stable) plaque psoriasis, and is characterised by well-defined, thickened, red plaques covered with silvery scales that are readily shed. A plaque is a raised patch on the skin more than 2cm across. If the scales are scratched or removed, characteristic pinpoint bleeding (Auspitz sign) is seen. Psoriasis plaques can occur almost anywhere on the body but the most commonly affected areas are the scalp, the extensor surfaces of the limbs (typically shins and elbows) and the lower back.
The plaques tend to be more or less symmetrical, which causes them to crack and bleed. A significant proportion of patients find their psoriasis lesions itchy. The extent of the disease is variable, ranging from a few plaques to more generalised disease covering large areas of skin.
Flexural psoriasis, scalp psoriasis and seborrhoeic psoriasis (sebopsoriasis) are the most common types of plaque psoriasis.
<h3><strong>Flexural psoriasis</strong></h3>
Flexural psoriasis (also known as inverse or intertriginous psoriasis) refers to plaque psoriasis affecting areas in the axillae groin, genital and natal cleft (between the buttocks) sites and under the breasts. Lesions are typically red, shiny and less scaly. They can also feel sore and be vulnerable to fungal infections.
<h3><strong>Scalp psoriasis</strong></h3>
Scalp psoriasis can vary, from light scaling, to grossly thickened scales stuck to the hair shafts. About 80 per cent of psoriasis patients will have some degree of scalp involvement. Profuse shedding of skin scales from the scalp can be a serious problem for some patients.
<h3><strong>Seborrhoeic psoriasis</strong></h3>
Seborrhoeic psoriasis is localised on seborrhoeic areas of the face, scalp and trunk. Some experts believe that infection with Malassezia yeasts (the ‘dandruff organism’) plays a role.
Other types of psoriasis are less common and are as follows: Guttate psoriasis (widespread, small scaly lesions); pustular psoriasis (yellow/brown-coloured sterile pustules on the palms of the hands or soles of the feet); and erythrodermic psoriasis (skin becomes reddened and inflamed all over the body).
<h3><strong>Pathophysiology</strong></h3>
The major biological abnormalities in psoriasis are as follows:
Hyperproliferation of the epidermis. This leads to thickening of the epidermis and scaling. Affected skin can be up to 16 times thicker than normal skin. The hyperproliferation is the result of larger-than-usual numbers of cells entering the growth phase, rather than acceleration of growth (ie, more cells growing rather than cells growing faster).
Abnormal differentiation (maturation) of keratinocytes. When the skin in psoriatic plaques is examined microscopically, the granular layer is missing, the <em>stratum corneum</em> is thickened and many of the cells in the <em>stratum corneum</em> still contain nuclei (normally lost by the time cells reach this layer).
Infiltration of the dermis and epidermis with activated T-lymphocytes and neutrophils.
Stimulation of the cutaneous vasculature, leading to new blood vessel formation in the psoriatic plaques.
Cell-mediated immune mechanisms appear to drive these processes. Activated T-cells release inflammatory cytokines that induce keratinocytes to release a number of compounds, including vascular endothelial growth factor (VEGF) and additional cytokines. A complex cascade of molecular events eventually results in keratinocyte proliferation, angiogenesis and neutrophil infiltration.
<h3><strong>Treatment</strong></h3>
<strong><em>Topical treatments</em></strong>
Topical treatments for psoriasis include emollients, topical corticosteroids, vitamin D analogues, coal tar and dithranol. NICE recommends that treatments are tried in a logical sequence until an adequate response is achieved.
For those prescribing and dispensing such treatment, it is important to counsel patients on application (for example, using assistance from another person to apply to hard-to-reach areas), to encourage the importance of adherence and to assess for cosmetic acceptability before supplying a given preparation. Equally, where a treatment has been deemed ineffective, it is important to clarify that application has been manageable, that adherence is high and that the patient does not have concerns about cosmetic acceptability of using the topical product that was prescribed.
All patients with psoriasis should be encouraged to use emollient therapy regularly, as frequently as they wish.
Emollients can help to increase the pliability of the skin surface and prevent skin-shedding. Emollients that contain humectants (eg, urea) are generally more effective and have longer-lasting effects.
Topical corticosteroids are effective for bringing flares of psoriasis under control. Other advantages of use include the fact that they are odourless and do not cause local irritation. However, the benefits of steroid use need to be balanced with the risk of local side-effects, such as skin atrophy.
Different product bases and preparations are generally needed, depending on the area of the body that is affected. For example, milder steroids are indicated for the face and flexures where skin is thinner, versus the trunk or limbs. Scalp-specific preparations are generally unsuitable to be used elsewhere on the body. Additionally, if more than 10 per cent of the body surface area is treated with topical corticosteroids, there is a risk of systemic side-effects.
<strong>Vitamin D analogues</strong>
Vitamin D and vitamin D analogues are most effective in combination with a topical corticosteroid. They act by inhibiting proliferation and promote differentiation of keratinocytes. In this way, they act to reduce the plaque-like quality of the skin and improve skin behaviour. They do not carry the risk of skin atrophy, so can be used more liberally. In fact, patients should be reminded that calcipotriol should be applied thickly, in contrast with topical steroid preparations. However, skin irritation, dryness and stinging can occur and accordingly, calcipotriol should not be applied to the face or flexures. Calcitriol is significantly less irritating and may be used in these areas.
<strong>Tar preparations</strong>
One of the longest-established treatments for psoriasis, coal tar’s mode of action is not well understood. Coal tar is believed to be keratolytic, with some anti-inflammatory and anti-proliferative effects. Coal tar stains clothing and is considered to have an unpleasant smell. It has been shown to be less effective than vitamin D derivatives. Crude coal tar contains a number of carcinogens and percutaneous absorption of mutagens is known to occur. Nevertheless, there is no epidemiological evidence that it increases the risk of cutaneous or internal cancers.
<strong>Dithranol</strong>
Dithranol has also been used for the treatment of psoriasis for many years. It is believed to exert a direct anti-proliferative effect on epidermal keratinocytes. It is a yellow powder that is profoundly irritating to normal skin and is not suitable for facial or flexural application. It causes temporary purple-brown staining of the skin. Long contact (12-to-24 hours) and short contact (15-to-30 minutes) applications are used. The paste is generally applied, followed by a tar bath and ultraviolet B irradiation. Generally, inpatient care is required.
<strong>Ultraviolet light-based treatments (UVB and PUVA)</strong>
Both UVB and UVA are thought to modulate the expression of cellular adhesion molecules and induce T-cell apoptosis. This interrupts the inflammatory processes of psoriasis. PUVA phototherapy involves the use of a topical or systemic psoralen sensitiser before UVA treatment. UVA therapy is used for plaque psoriasis and palmoplantar pustular psoriasis. Phototherapy is used for those with plaque or guttate pattern psoriasis that cannot be controlled by topical treatments. Treatment is administered two or three times weekly. Unfortunately, UV light therapy tans the skin and presents a dose-related increased risk of skin cancer.
<strong>Systemic non-biological treatment</strong>
Immunomodulatory agents such as methotrexate, cyclosporin and acitretin are sometimes used where response to other therapies is unsuccessful. The risk of adverse effects always has to be weighed-up against the benefits with these treatments. Methotrexate is the treatment of choice, followed by cyclosporin if not tolerated. Apremilast has recently been approved for reimbursement under the HSE PCRS and is a new oral selective PDE4 inhibitor. It acts early along the inflammatory signalling cascade. The dose is up-titrated over the first week to minimise GI side-effects. Unlike the other agents, apremilast does not require therapeutic monitoring.
<strong>Biological treatment</strong>
A number of biologic agents have been licenced for the treatment of psoriasis, including the established TNF inhibitors (eg adalimumab, etanercept and infliximab), the interleukin (IL)-12/23 compound ustekinumab, and the IL-17A antagonist, secukinumab.
In more recent years, ixekizumab (a humanised, anti-IL-17 monoclonal antibody) has become available for the treatment of moderate to severe plaque psoriasis in adults who are candidates for systemic therapy.
The most recent agent to be reimbursed in Ireland (May 2018) is guselkumab, which selectively targets IL-23, for the treatment of adults with moderate to severe plaque psoriasis who are candidates for systemic therapy.
These agents have significantly broadened the range and efficacy of treatment options available for more severe psoriasis patients.
<div style=”background: #e8edf0; padding: 10px 15px; margin-bottom: 15px;”>
The Irish Skin Foundation (ISF) is a national charity with a mission to support people with skin conditions. The charity operates a helpline, provides up-to-date specialist guidance, information booklets and resources, runs events, awareness campaigns, and engages in advocacy for people with skin conditions.
The ISF Helpline is open Monday to Friday, 10am-4:30pm, to answer general e-mail or phone queries. The service is completely free.
The ISF has recently published a revised and expanded psoriasis patient support booklet, <em>What you need to know about psoriasis</em>, which is a useful resource to give to patients with psoriasis. It is available free of charge by post or can be downloaded from the ISF website at www.irishskin.ie.
As part of Eczema Awareness month, the ISF will host a free public meeting in the Red Cow Moran Hotel, Naas Road, Dublin, on 29 September for those with, or caring for someone with, eczema.
This Eczema Expert meeting is the third ISF annual meeting for people living with or caring for those with eczema. Details at <a href=”http://www.irishskin.ie”>www.irishskin.ie</a>.
</div>






Leave a Reply
You must be logged in to post a comment.