Dr Rachel Cole and Prof Geraldine McCarthy discuss optimum gout management
Case report
A 72-year-old man was admitted to hospital in March 2019 with heart failure secondary to new onset atrial fibrillation. He had a past history of hypertension and chronic kidney disease (CKD) stage 3. He had had one episode of acute first metatarsophalangeal (MTP) arthritis associated with hyperuricaemia four months previously and had been prescribed allopurinol for presumed gout at that time, although without colchicine prophylaxis.
Upon admission, he commenced treatment with intravenous furosemide, bisoprolol and edoxaban with slow clinical improvement.
Two weeks following admission, he developed severe right-sided knee pain and swelling that also occurred on the left side two days later. Temperature was 37.9 C0, C-reactive protein (CRP) 226mg/L, and serum urate 227umol/L. He was treated with intravenous antibiotics for presumed septic arthritis. He underwent an ultrasound guided knee aspirate, which was culture negative. He proceeded to have bilateral arthroscopic washouts for presumed septic arthritis. Joint fluids obtained were also culture negative, so he was treated as culture-negative septic arthritis.
The rheumatology service was then consulted two days later and spun joint fluid samples were retrieved from the microbiology laboratory and examined by polarised light microscopy. Large quantities of both monosodium urate (MSU) and calcium pyrophosphate dihydrate (CPP) crystals were identified. Allopurinol 300mg once daily was continued and colchicine 0.5mg twice daily was added. At that time he was having difficulty mobilising due to residual joint contractures, effusions and muscle wasting from immobility during the preceding weeks. To accelerate recovery, both knees were aspirated and injected with triamcinolone acetonide 40mg and 2cc 1 per cent lidocaine with rapid improvement in symptoms and gradual increase in mobility.
Gout has been on the
minds of clinicians since 2,640 BCE, when it was first described by the
Egyptians. It was described as “the king of diseases and the disease of kings”,
and George Eliot wrote that the rich “accepted gout and apoplexy as things that
ran mysteriously in respectable families”. Uric acid runs higher in primates,
which may have conferred an evolutionary advantage due to anti-hypertensive and
anti-oxidant properties.
Gout is a chronic disease of deposition of monosodium
urate (MSU) crystals and is the commonest form of inflammatory arthropathy,
with a prevalence of 3-6 per cent in men and 1-2 per cent in women in Western
developed countries. While there is a three times higher prevalence in men,
this gender difference declines after menopause. Some ethnic groups, such as
the Taiwanese Aborigines, the Maori, and the Pacific Islanders, have a
prevalence more than two times greater than that of other ethnic groups. The
clinical manifestations occur as a response to MSU crystals, which form in the presence
of increased serum urate concentrations. Effective treatment is achieved by
therapeutic strategies that result in dissolution of MSU crystals.
Comorbidities are common in people with gout. These include hypertension, chronic kidney
disease (CKD), obesity, diabetes, myocardial infarction and stroke. Gout is
associated with reduced risk of neurological disorders such as Parkinson’s
disease, Alzheimer’s disease and both vascular and non-vascular dementia.
Extracellular urate may have neuroprotective or antioxidant properties, as
serum urate concentrations have an inverse association with Parkinson’s disease
and dementia.
Gout costs in the US are estimated at $27 million
annually. It carries a high personal burden: Work loss rates are similar to
rheumatoid arthritis (RA). In contrast to RA, hospitalisation rates have
doubled in the last 20 years. Globally the disability-adjusted life year (DALY)
burden has increased by 49 per cent in gout sufferers.
Dietary risk factors for hyperuricaemia and the development
of gout include alcohol, red meat, seafood, and sugar-sweetened beverages.
Intake of vitamin C and low-fat milk can reduce serum urate levels. Diuretic
use is an important risk factor for hyperuricaemia and development of gout.
Pathology
Increased urate
concentration leads to chronic deposition of MSU crystals. The clinical
features of gout arise due to the inflammatory response to crystals.
Pathological hyperuricaemia is a level greater than 380 umol/L. Above this
level, MSU crystals form in vitro. Hyperuricaemia results from increased
hepatic production, reduced renal excretion, or both. Of note, of all patients
with asymptomatic hyperuricaemia, only about 15–20 per cent will develop gout.
The ‘clinical gout’ response is initiated when MSU
crystals interact with resident macrophages to form and activate the NLRP3
inflammasome. The inflammatory response is amplified by activation of
neutrophils and mast cells, leading to the release of a host of
pro-inflammatory cytokines.
Variability in the solubility of urate in the joint
fluids may explain why gout favours the first metatarsophalangeal (MTP) joint
(a peripheral joint with a low temperature) and why attacks occur at night
(intra-articular dehydration).
The progression of gout can be defined by four pathophysiological
stages: hyperuricaemia without evidence of crystal deposition or clinical gout;
crystal deposition without symptomatic gout; crystal deposition with
symptomatic gout; and advanced gout (tophi, chronic gouty arthritis, and
radiographic erosions).
Clinical manifestations
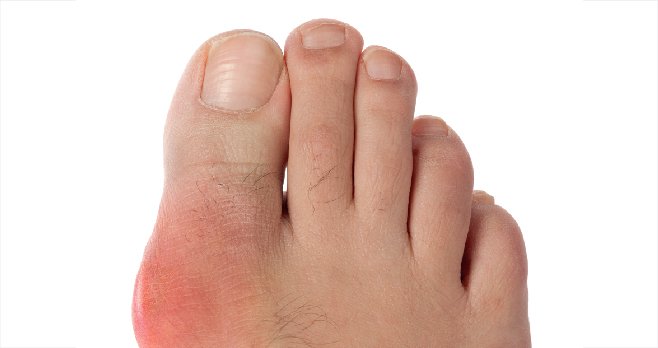
Acute gouty arthritis
commonly presents initially in the first MTP joint, foot or ankle. Pain is
typically of rapid onset, severe and associated with erythema, swelling, heat,
exquisite tenderness and joint immobility. Triggers for flares include acute
medical or surgical illness, dehydration or dietary factors such as alcohol
intake or purine-rich foods. Flares
often occur at night.
An acute attack is typically a self-limiting episode
lasting one-to-two weeks. There is complete symptom resolution in the
‘intercritical period’. Persistent hyperuricaemia leads to recurrent gout
flares with increasing frequency, which are more prolonged and can become
polyarticular, including joints of the upper limbs.
If hyperuricaemia remains untreated, advanced gout
with tophi or chronic gouty arthritis can develop. The pathognomonic feature of
chronic gout is the tophus, which is an organised granulomatous response to
crystal deposition. Tophi are frequently seen in the helix of the ear, the
olecranon processes, Achilles tendons, toes, fingers and knees. They are
painless and occasionally get infected. Advanced gout is characterised by
chronic joint pain and deformity, structural joint damage, frequent flares and
functional limitation.
Examination will show evidence of synovitis with
marked tenderness, erythema, swelling and increased temperature of the skin
overlying the affected joint. Fever can occur, particularly with polyarticular
flares. The initial attack is occasionally polyarticular (3-14 per cent), and
acute attacks rarely affect the shoulders or hips.
Diagnosis
The gold standard for
gout diagnosis is confirmation of MSU crystals by polarising light microscopy
(PLM) of synovial fluid or tophaceous material. Volumes as small as one drop of
joint fluid may be sufficient to make the diagnosis. Ideally, samples should be
examined within six hours, but can be refrigerated and examined later if
necessary. MSU crystals appear as strong negatively birefringent crystals
against dark background. They appear yellow when aligned parallel to the axis
of red plate compensator. Acute gout and septic arthritis can co-exist. During
an acute flare, synovial fluid appears cloudy, and will have a high white cell
count of over 50,000 in some cases. Therefore, fluid should also be sent for
gram stain, culture and sensitivity.
Most people with hyperuricaemia do not have gout, so
hyperuricaemia alone is insufficient to make a diagnosis. However, individuals
with uric acid levels persistently below 360umol are unlikely to have or be at
risk of developing gout. Importantly, one-third of acute cases have a normal or
low serum urate at presentation.
CRP can be as high as in excess of 100mg/L. There can
also be a neutrophil leucocytosis. These are non-specific findings.
Radiographs will be normal or show soft tissue
swelling. Bone erosion is seen with advanced gout, characterised by a sclerotic
rim and overhanging edge representing bony tophus. Ultrasound will show a
double contour sign over the surface of the joint cartilage or a ‘snowstorm’
appearance of crystals within the synovial fluid. CT is not helpful in the
diagnosis of acute gout, as it cannot detect inflammation, synovitis,
tenosynovitis and osteitis. However, dual energy CT (DECT) is a method of CT
imaging that, by analysing the difference in attenuation in a material exposed
to two different x-ray spectra, can identify and help quantify urate deposits
in patients with gout.
The Study for Updated Gout Classification Criteria
(SUGAR) considered that there is frequently difficulty accessing the gold
standard PLM, particularly in primary care, so ten key features were proposed
to discriminate gout from other similar presentations. They are: (1) joint
erythema, (2) at least one episode involved difficulty walking, (3) time to
maximal pain less than 24 hours, (4) resolution by two weeks, (5) tophus, (6)
first MTP joint involved, (7) location of currently tender joints, (8) serum
urate level over 360umol, (9) US double contour sign, and (10) radiographic
erosion or cyst.
The key differential diagnosis is septic arthritis,
which as mentioned can co-exist with gout. Other forms of inflammatory
arthritis can mimic gout, in particular acute CPP arthritis (‘pseudogout’). It
is unknown how often acute crystal arthritis is presumed to be
‘culture-negative septic arthritis’ alone when joint fluid is not examined
under polarised light, either because PLM is not available or because the
clinician has not initially considered the diagnosis, as occurred in the case
described in this article. This scenario can lead to unnecessary antibiotic
therapy and/or surgical procedures.
Treatment
Options for treatment
of an acute flare include non-steroidal anti-inflammatories (NSAIDs),
colchicine, or corticosteroids, which can be administered orally,
intra-articularly or, less frequently, parenterally. Chronic treatment strategy
focuses on MSU crystal dissolution. Urate-lowering therapy (ULT) is indicated
for people with recurrent flares (more than one flare per year), tophi, and/or
stage 2 CKD. British guidelines advise to wait one-to-two weeks after a flare
to start ULT, but the American guidelines support an immediate start.
Two studies have shown that starting ULT during a
flare does not prolong it provided it is being adequately treated. Crystals
mobilise when they begin to dissolve in response to ULT and can shed into the
joint space, triggering inflammation. Slowly uptitrating ULT reduces the risk
of it triggering a flare.
Most importantly, ULT should not be discontinued at
the onset of and during a gout flare occurring while a patient is receiving
ULT. It should be simply continued at the current dose and the flare should be
managed appropriately
Prevention of acute flares during the first
three-to-six months (due to crystal mobilisation) of ULT can be prevented with
the use of colchicine or low-dose NSAIDs daily. Such prevention is extremely
important, as without it, the increase in gout flares that occur upon
initiation of ULT will likely induce the patient to discontinue it. Colchicine
is the preferred agent and some individuals, particularly those with a large
crystal burden (eg, multiple tophi), will require colchicine prophylaxis for 12
months or longer.
The therapeutic target urate is 360umol/L in
non-tophaceous gout and 300umol/L in tophaceous gout. ULT doses should be
adjusted upwards with monthly serum urates until the therapeutic target is
reached, after which the serum urate should be checked every six months to
ensure compliance and appropriate dosing.
There are three main classes of ULT. Xanthine oxidase
inhibitors (allopurinol and febuxostat) inhibit urate production. Uricosurics
(probenecid and lesinurad) increase renal urate excretion. Recombinant uricases
(rasburicase and pegloticase) catalyse the conversion of urate to allantoin.
Colchicine and allopurinol remain the staple
first-line treatments for flares and prophylaxis, and prevention, respectively.
Febuxostat is an alternative, particularly in those in whom allopurinol cannot
be used although only two doses are available in Ireland, 80mg and 120mg. In
some patients, the minimum dose of 80mg may drive the serum urate lower than
necessary or desirable. The uricosuric probenecid can be prescribed alone or in
combination with xanthine oxidase inhibitors. Lesinurad is not currently
available in Ireland. Recombinant uricases are administered by intravenous
infusion in a hospital setting.
Allopurinol hypersensitivity syndrome is the most serious
potential adverse event. It usually happens within the first two-to-three
months, is made more likely by diuretic use, and is an indication to
discontinue the treatment. It is also more likely in Koreans, Chinese, and
patients with renal failure. It presents with a desquamating rash, hepatitis,
abnormal renal function, and eosinophilia. An estimated 2 per cent of those
receiving allopurinol will develop a mild rash.
In terms of drug alternatives to reduce risk of gout
attacks, it is recommended to continue diuretics for heart failure but not
hypertension. Spironolactone should be advised where possible. Consider
fenofibrate for hypercholesterolaemia. Calcium channel inhibitors and losartan
should be prescribed for hypertension.
Of note, cardio-protective aspirin modestly increases
uricaemia by inhibiting urate excretion. This is not a contra-indication to its
use, however. Azathioprine should not be co-prescribed with xanthine oxidase
inhibitors as the concentrations of its metabolite 6-mercaptopurine are
increased leading to myelosuppression.
Allopurinol and colchicine are also safe in CKD with
cautious dose escalation being shown to be well tolerated in these patients
Of concern, only 30-60 per cent of patients are still
taking allopurinol a year following initiation, while 40 per cent are receiving
suboptimal dosing failing to reach their therapeutic target. Just over half, 53
per cent, of GPs and 35 per cent of rheumatologists exhibit low adherence to
treatment guidelines.
Conclusion
In conclusion, gout
is a treatable disease and the strategy of long-term lowering of serum urate
concentrations is highly effective. Despite this, the prevalence of gout
continues to increase and many patients have very poorly controlled disease.
Enhanced education of both medical practitioners and patients could lessen
confusion and lead to improvement in diagnosis, treatment as well as compliance
with therapy. This in turn would improve long-term outcomes in this highly
treatable disease.
References on request





Leave a Reply
You must be logged in to post a comment.