Almost a year after the implosion of GP representative body the NAGP, Niamh Cahill and Priscilla Lynch examine the colourful history of the organisation and where its legacy lies
In July 2013 a new GP representative organisation, the National Association of General Practitioners (NAGP), burst onto the scene. The NAGP, based on the defunct Association of GPs (AGP), promised to be a strong new independent voice for general practice at a time when GPs were struggling with the impact of FEMPI cuts. Its launch followed the controversial departure of IMO CEO Mr George McNeice from the Organisation with a huge pension pay-out of almost €10 million at the end of 2012, which led to a large number of GPs resigning from the union.
The NAGP quickly established itself as very media-friendly, with regular press releases, strong spokespeople and a number of high-profile campaigns. The Association’s CEO throughout its existence, Mr Chris Goodey, had a background in medical publishing and the pharmaceutical industry and knew how to garner media coverage and arrange successful largescale events.

The NAGP’s membership grew steadily as its profile increased. Within a year it claimed to have 1,000 members, climbing to an eventual 2,000, though this figure was often questioned.
Some of its critics who spoke to the Medical Independent (MI) for this article say the NAGP’s approach was contradictory and rash on some matters, particularly in “playing the political game”, while supporters praised its passionate, up front approach. The latter group felt that having a representative organisation dedicated solely to general practice was a big advantage.
The NAGP quickly established itself as very media-friendly, with regular press releases, strong spokespeople, and a number of high-profile campaigns
From the outset, the NAGP pushed a strong agenda of ‘general practice is in crisis’, with numerous meetings, press releases, and calls for a national 10-year cross-party ‘Tallaght strategy’ on the health service, which sowed the seeds for Sláintecare. The NAGP was also largely behind the success of the #nodoctornovillage campaign, which saw the election to the Dáil of Independent candidate in Clare, GP Dr Michael Harty (who was a member of both the IMO and NAGP).
Under-sixes debacle
From the beginning, the NAGP was determined to plough its own path, and differed from the IMO in its response to various Government healthcare initiatives involving general practice. For example, in October 2013, the NAGP welcomed the then Government’s announcement on the provision of free GP care for all children under five years of age.

Speaking at the time, Dr Andy Jordan, Chairman of the NAGP said: “The decision to introduce an under-fives care scheme is greatly welcomed by the NAGP. It is a great visionary step for healthcare in Ireland similar to the 1950s when the then Health Minister, Noel Browne TD, introduced a mould-breaking Mother and Child Scheme, which was to provide free medical care for all expectant mothers and their children up to the age of 16 years.”
However, the NAGP soon changed its tune when it saw the budget allocation (€37 million) for the initiative, and issued a series of press statements strongly criticising the Government over the move. When it came down to negotiating the terms of this new contract, only the IMO was involved and the NAGP soon took a back seat.
The NAGP strongly opposed the eventual deal struck between the Government and the IMO early in 2014 and supported members in rejecting the contract. It issued member survey results that were negative about signing up to the new contract and held large well-attended GP meetings at a very difficult time for general practice in Ireland, as GPs struggled with income cuts under FEMPI. Also many GPs felt pressurised to accept the under-sixes contract to keep their patients despite the increased workload.
In May 2014 the NAGP also issued a very critical statement about the IMO following its agreement with the then Competition Authority (now the Competition and Consumer Protection Commission, CCPC) in the High Court regarding the issue of collective negotiations.
“The IMO has been asleep for 10 years,” said Mr Goodey at the time. “The NAGP re-launched itself last July and suddenly the IMO woke up. As a result, the NAGP decided to give the IMO the benefit of the doubt and gave them our full support regarding the High Court Competition Authority case and many other issues affecting general practice. It is time that GPs unite under one umbrella organisation – the NAGP,” Mr Goodey added. “At all times the aim of the NAGP is to ensure better outcomes for general practice patients.”
While there had been tension between the two organisations from the beginning, now it was all-out hostility and a further critical NAGP press release cemented the ill-will.
The IMO consistently pointed out that it was the only union with a trade union negotiating license that could represent GPs in national agreements with the Government.
While in 2014 the NAGP announced it had secured a negotiating license via an arrangement with the Independent Workers Union of Ireland and was optimistic it would enable the Association to take part in contract negotiations, this never came to fruition. The Government signed up to a memorandum of understanding with the IMO on GP contract negotiations following resolution of the CCPC issues and alleged the NAGP did not have affiliation with the Irish Congress of Trade Unions and could not be a formal party to such negotiations.
While the HSE did engage with the NAGP on a range of general practice-related issues, including the pre-general election rural practice deal agreed by the Government in 2016, the NAGP’s absence from official negotiations on contract issues would remain a major stumbling block for its members until its demise in 2019.
Former Minister for Health Leo Varadkar gave the NAGP a cold shoulder following the under-sixes contract stand-off, despite strong pressure from NAGP members and conciliatory overtures from the Association.
However, the next Minister for Health Simon Harris took a more diplomatic approach and eventually invited the NAGP to the table on what was claimed to be a new GP contract. But, it was very clearly stated by its rival that the NAGP was only involved in “discussions and consultation as opposed to real negotiations”.
The NAGP also tried to reconcile with the IMO and made several public and private attempts to get the two organisations to work together or provide a united front, which were rebuffed by the IMO.
Financial issues
Running a trade union is not cheap. From the outset the NAGP set its membership rates lower than the IMO, and despite constant pleas to the HSE, it was not able to have its fees deducted through the HSE GMS payments system, like its rival union. Thus the NAGP was always “chasing” members for fee payments, which created cash flow issues, according to one former senior member.
As the scope of its work increased, and it expanded its services and staff numbers, the NAGP needed more cash and set up a ‘fighting fund’ for dealings with the CCPC, where it aimed to raise €1 million. The fund, made up of GP donations of about €1,000 each, continued to raise money through 2015 and in early 2016 it was revealed it had raised only €164,000.
In March 2018 the NAGP commissioned an independent audit and statement of affairs in relation to its legal fund, according to a statement released to members, following growing queries about how the money had been spent.
Up to this point, €220,000 has been spent by the NAGP on legal campaigns, legal advice and the under-sixes injunction, according to the statement. The NAGP carried out four campaigns over two years, including legal preparation against the CCPC; a campaign to highlight competition law; injunction proceedings against the HSE to prevent the removal of patients from GMS panels of those GPs who did not sign the under-sixes contract; and nationwide roadshows regarding the under-sixes contract.
“The preparation process and the legal actions, along with the campaigns, were extremely expensive and as such we felt it was necessary to raise a fighting fund of €1 million to support our endeavours. This was the estimate suggested by William Fry Solicitors needed to fight a High Court case. We fell well short of this, raising only €164,000,” the statement outlined.
Spin-off ventures
The NAGP also became involved in spin-off financial ventures, with varying successes. A number of events such as the Primary Care Partnership conferences and charity galas attracted large attendances and sponsorship. Between April 2017 and March 2018 the NAGP received €80,000 in pharmaceutical and “other service provider” sponsorship, Mr Goodey said in a statement to members. The money was used to cover the cost of meetings and roadshows.
Possibly the most noteworthy financial spin-off the NAGP became involved with was GP Online, which came about at a time when a number of private online and telemedicine GP service providers began springing up in Ireland.
The IMO voiced its opposition to such services, saying they were no replacement for holistic primary care and were open to abuse, while the NAGP took a different tack.
In January 2016, MI revealed details of the NAGP’s new GP telemedicine service. The GP Online app was to support face-to-face video consultations and the production of prescriptions between GPs and their own registered patients. It was due to be rolled out nationally before the end of that year. The NAGP owned a percentage of the business, though this percentage went from a majority to minority stake over time.
The app was heavily promoted to NAGP members and the media and investors were sought, while the Association held discussions with the HSE about potentially being paid to allow medical card patients use the app to access their GP.
The NAGP also announced in June 2016 that it was going to launch its own ambitious GP practice management software package, which was to use cloud-based technology and cover both private and GMS patients. It was claimed it would be better than what the current providers offered.
However, delays soon occurred and promotion of the app and software package stopped.
In 2018, Mr Goodey assured GPs that teething problems regarding the development of GP Online would be fully addressed. Mr Goodey, then also the CEO of GP Online, explained that following a six-month pilot with 20 GPs, feedback revealed the system was not user-friendly on the GP side.
“For patients it was very easy to use but for GPs the technology was quite clunky so we basically had to redevelop the software,” Mr Goodey explained. He told this newspaper in 2018 that the vast majority of investors in the company were GPs, with “six or seven” non-GP investors.
The NAGP owned 6.9 per cent of GP Online at that stage, Mr Goodey added. He said in the next three years the company hoped to raise €3 million from institutional investors and that €1 million had been spent in getting the company to where it was at that stage. However, the venture quietly disappeared.
A GP who invested in the GP Online project, who spoke to MI, explained that the venture sounded “like a no-brainer” at the time. The GP explained that despite seeking information on their investment on countless occasions, they were never given any details of developments.
The company traded as GP Online, but its official name in company records was Millenium Medical Solutions Ltd. It was placed into liquidation in July 2019. A separate company, with the same Kildare Street address as the NAGP, Millenium Medical Solutions Nominees Ltd, was dissolved in September 2019.
MSC Eurocare
Another high-profile project the NAGP became involved with was its promotion of the European Cross Border Healthcare Directive (CBD). The CBD was introduced in 2014, offering patients the option of receiving healthcare in another European country and having it reimbursed by the HSE.
In 2014, when the scheme was first introduced, just 148 Irish patients availed of healthcare under the directive. In 2016, the figures had jumped dramatically, with 1,025 patients using the scheme at a cost to the HSE of €2.5 million. Joint replacements and cataract surgery were among the most frequently reimbursed procedures under the directive. HSE spending on the CBD increased exponentially during 2017 and 2018 as increasing numbers of patients sought to avail of the scheme.
In July 2017, the NAGP announced its intention to highlight information about the CBD due to huge waiting lists for public hospital outpatients and surgical procedures nationally.
The NAGP developed a poster and leaflet for GP surgeries with information on the CBD in a bid to increase awareness among patients and GPs. The leaflet was produced with the support of Age Action; IMED Hospitals, Spain; Kingsbridge Hospital, Belfast; St Joseph’s Hospital, Wales; and MSC Eurocare.
MSC Eurocare was a newly established company offering assistance to patients who sought to use the CBD. The company arranged treatment for patients under the directive, including transport, hospital appointments, etc, and provided a short-term loan to patients, if required, to pay for treatment. The loan was repayable when the HSE refund for the cost of the treatment was issued, usually within 28 days of receipt of application.
MSC Eurocare had “partner hospitals” or specifically selected hospitals that it directed patients towards when seeking healthcare abroad under the directive. A number of NAGP officials travelled to these and other hospitals abroad, as part of the NAGP’s information campaign on the directive.
Dr Jordan, speaking as NAGP Chairman, said Association members had travelled to the Kingsbridge Hospital; the UK; Spain; North Wales; Portugal; and France to examine hospitals “on the ground”.
Dr Jordan stressed that no payment between the NAGP and hospitals abroad had taken place, despite a number of private hospitals being named on the NAGP information leaflet.
Dr Jordan stressed that the real purpose of the campaign was to promote the scheme itself and not individual hospitals. Mr Goodey also emphasised that no payment or exchange of money had taken place between the NAGP and recommended hospitals.
MSC Europe, which it later transpired shared links with the NAGP, eventually dissolved in December 2019.
The beginning of the end
In late 2017 cracks began to appear in the NAGP’s public image and concerns began to emerge from some NAGP council members regarding finance and governance. A rising deficit was among the first alarm bells sounded, causing some concern among ordinary members.
A five-figure deficit (€33,000) was mentioned in the early 2017 AGM report and this was raised by a member at the AGM. It turned out staff pay at the NAGP for an average of three employees over a 15-month period was more than €300,000, according to its abridged financial statements from 1 January 2016 to the end of March 2017.
The statements also revealed that income totalled €835,000 for the 15-month period compared to administrative expenses of €895,000, amounting to an overspend of around €60,000. But the income included almost €190,000 in debtors, largely made up of unpaid “membership and sponsorship”, which would mean that actual income was €645,000.
This was only the beginning, however, and the NAGP’s financial issues would continue to escalate until it became completely insolvent.
Abridged financial statements for the NAGP for the year ending 31 March 2018 revealed a deficit of more than €114,000. The figure represented a significant increase based on financial statements for the end of March 2017, which showed a deficit of €33,000.
Over the course of late 2017 and early 2018, a number of NAGP council members had been raising concerns and seeking answers on a number of issues. Frustration grew as questions were dismissed and went unanswered. As originally revealed by this newspaper, in early 2018 the NAGP lost six council members, including the then incoming President Dr Yvonne Williams. Many of these members raised concerns about financial and governance issues, and potential conflicts of interest within the Association. Some former high-profile spokespeople for the organisation quietly began to back away from the NAGP.
Following a report into governance arrangements at the Association, a number of changes were recommended. Remaining council members for months tried in vain to introduce the recommendations, while the Association continued its work for GPs, issuing press releases and hosting meetings, but to no avail.
A “whistle-blower” document making a number of astonishing claims about the NAGP and some of its officials came into circulation in 2018, adding further fuel to the fire of negativity surrounding the Association.
Endgame
While the NAGP was clearly in a lot of trouble by the start of 2019 and there were serious doubts it could continue, it did manage to organise a large high-profile GP protest outside Dáil Éireann in early February 2019.
At the protest, almost 500 GPs (according to the NAGP) expressed their anger at the state of the health service and the destruction of Irish general practice, which garnered favourable public support and media coverage. The protest was followed by the release of a poll of NAGP members, which claimed 94 per cent of the respondents had no confidence in Minister Harris. It was to be the last hurrah for the NAGP.
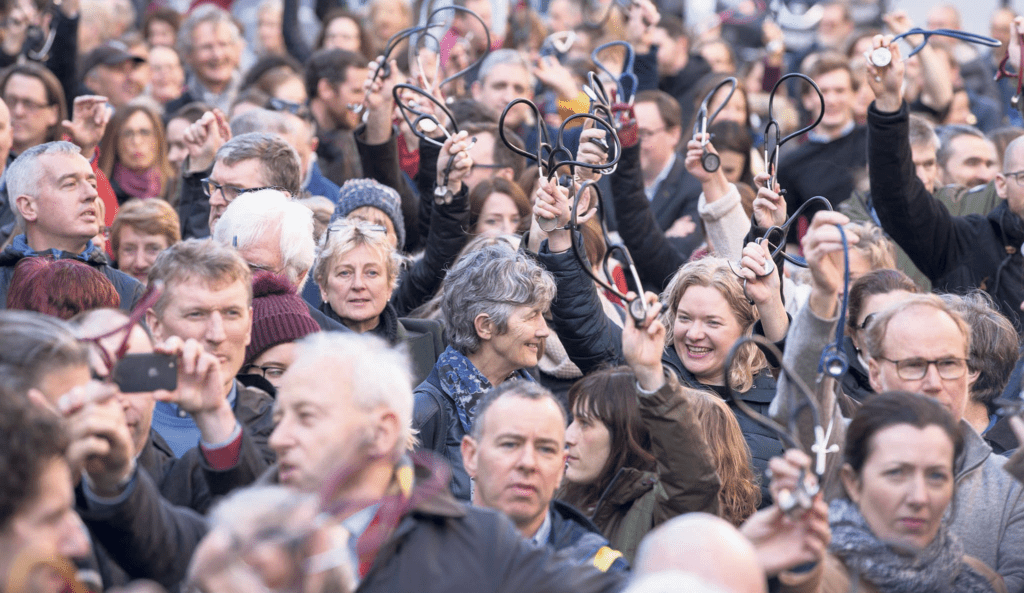
In April that year, businessman Mr Chay Bowes delivered a report to NAGP directors and council members into financial governance and operations. The contents of the report, former NAGP members would later reveal, left them aghast.
Mr Bowes reported several cash drawings associated with Mr Goodey, beyond his annual salary of €120,000. Mr Goodey strenuously denied any impropriety and claimed all expenses were related to legitimate NAGP business.
The Bowes report outlined that €250,000 in membership fees were owed in 2019, but added that because of poor financial practices at the Association, it was unclear whether this figure was accurate.
The report’s revelations drew negative media coverage and shock from the NAGP council members and the general membership. On Sunday April 28, 2019 came an announcement that the entire national council had resigned, including then NAGP President Dr Maitiú Ó Tuathail amid serious concerns about internal governance.
This news came as a bombshell to many GPs across Ireland, who had been paid-up members of the NAGP for years and despite the rumours of difficulties, felt left in the dark about its demise.
A statement to the NAGP membership by the council upon its resignation, seen by MI, stated that concerns were raised at the 2018 AGM about governance at the Association.
“Following this, the national council commissioned a governance report from Ampersand, which recommended a new governance structure for the organisation, and we had begun that journey,” the statement read.
“Subsequently, serious issues of internal governance were brought to the attention of the national council and the directors of the NAGP.
“Significant efforts were made to resolve these issues through a process of renewal, transparency, and accountability. We regret and apologise to our members that this was not achieved. As a result, the national council, whose role is advisory, have tendered their resignation to the directors.”
The statement concluded: “We believe in general practice, our membership and above all in integrity. We plan to continue to support you and will issue further correspondence soon.”
In a separate statement to members from the NAGP, also issued to members, the organisation said the directors, who included Drs Jim Stacey, Andy Jordan, and Chris O’Rourke, would “strive to ensure a rescue package will be in place within the next two weeks which will facilitate the continuation of the organisation and implement the recently commissioned governance report”.
The above was the only reference to governance in the statement, which also referred to the recent GP deal on the reversal of FEMPI cuts brokered between the IMO and Department of Health. The statement criticised the Government for failing to allow the NAGP to sit at the “negotiating table” and claimed the IMO and Department enjoyed “a cosy relationship, which in effect could be considered illegal State aid”.
In reference to ongoing financial challenges, the statement noted: “Many GPs are waiting to see the details of the new offer [IMO GP deal] before they renew their membership subscription. This has created financial difficulties for the NAGP.”
Rescue package
Following the council resignations, the bleak financial picture at the NAGP became apparent. Mr Goodey and the directors began efforts to secure a “rescue package” to save the organisation from ruin.
However, the NAGP finally entered into voluntary liquidation in May 2019. In an official member update from NAGP Directors Drs Jordan and Stacey, it was announced that the trade union’s holding company (NAGP) had entered voluntary liquidation with “regret and a heavy heart”.
The “business part” of the company was wound up, while the union, known as the Alliance of Family Doctors (AFD), would continue to operate and “may be joining one of the large trade unions”, the doctors announced.
The NAGP took no responsibility for the collapse of the Association, despite the governance and financial issues highlighted in the Bowes report, and instead blamed the negative media coverage for its downfall.
It was claimed that prior to what it called “leaks” and “adverse publicity” in the media, that Mr Goodey had managed to secure a rescue package of €200,000 from “well-wishers” of the NAGP, which would have been “enough to pay all creditors” and ensure viability.
“Unfortunately that rescue package collapsed after the negative media coverage. Had that particular article not run, the rescue package was there and we could have paid all our creditors”.
“The negative publicity has effectively left us facing insolvency.”
The statement failed to outline, however, what in the media coverage was untrue and did not address the governance and financial concerns raised by former members. The findings of the independent financial reports were forwarded to the Office of the Director of Corporate Enforcement (ODCE) and the gardaí.
Gone but not forgotten?
Following the collapse of the NAGP, talks commenced on moving the membership to the union Unite. In August 2019 a deal was struck with Unite, which said it was to advocate on behalf of the AFD.
The AFD announced that the agreement would give members a stronger, more powerful voice in the future. Since then, however, very little has been heard from the alliance and former members of the NAGP have not received any updates, it is understood.
Over the course of late 2017 and early 2018, a number of NAGP council members had been raising concerns and seeking answers on a number of issues. Frustration grew as questions were dismissed and went unanswered
The alliance has no website and its official Twitter account has not featured any updates related to the alliance for some time.
Dr Jordan, former Chairman of the NAGP, is Director of the AFD. At the time of going to press, he had failed to respond to calls seeking an update on the organisation.
Regarding the investigation of the NAGP by the ODCE, the office said it does not comment on cases and failed to provide an update.
In relation to an alleged Garda investigation, a spokesperson for An Garda Síochána told MI: “We had received similar queries in 2019. We have received confirmation that there has been no change in status. There is no investigation at GNECB [Garda National Economic Crime Bureau] related to the National Association of General Practitioners.”
MI approached a number of senior members of the NAGP to be interviewed for this feature. All either declined to speak on the record or didn’t respond to our requests for an interview.
Some former members, however, spoke fondly of the positive impact they felt the NAGP had on raising and promoting general practice issues nationally. They praised the many talented, hardworking council members who, they said, had a real, and now largely unappreciated impact on resolving issues with the HSE and Government and “were important voices for general practice”.
As one former member concluded: “Well whatever the NAGP’s faults, it was never boring!”













Leave a Reply
You must be logged in to post a comment.