New international clinical practice guidelines have been published for the diagnosis and management of von Willebrand disorder (VWD). Despite being the most common inherited bleeding disorder, with approximately onein-1,000 of the population being affected, VWD is underdiagnosed, undertreated and under-recognised, and in many countries the proportion diagnosed stands at between 10 and 20 per cent.
The new VWD guidelines aim to improve diagnosis and treatment of VWD and were drawn up by the American Society of Hematology (ASH), the International Society on Thrombosis and Haemostasis (ISTH), the US National Hemophilia Foundation (NHF), and World Federation of Hemophilia (WFH), and are published in the journal Blood Advances. Two expert panels made up of international hematologist, people living with VWD and scientists with expertise in appraising clinical evidence developed the guidelines.
They started by identifying the most important clinical questions about VWD diagnosis and treatment through an international survey and panel discussions. This was combined with a systematic review of all available evidence about VWD, conducted by the University of Kansas Medical Center, US, which the panel referred to when making its recommendations.
The finalised guidelines detail 19 recommendations on diagnosis and management of VWD Key recommendations include the role of bleeding-assessment tools in the assessment of patients suspected of VWD, diagnostic assays and laboratory cut-offs for type 1 and type
2 VWD, how to approach a type 1 VWD patient with normalised levels over time, and the role of genetic testing vs phenotypic assays for types 2B and 2N. Future critical research priorities are also identified. For the first time, it is recommended that VWD patients who suffer from frequent, severe bleeding that decreases their quality-of-life should receive routine VWD prophylaxis, an injectable concentrate of clotting protein, several times a week.
Specific regimes are recommended for the treatment of heavy menstrual bleeding with tailored treatment depending on whether or not the woman may wish to conceive. The establishment of multidisciplinary clinics to include a haematologist and gynaecologist to optimally diagnose and treat women with VWD is also recommended. The guidelines also call for the classification of VWD to be more inclusive of patients who experience bleeding, but whose blood tests do not meet currently accepted thresholds for diagnosis.
Dr Martin Tallman, from Memorial Sloan Kettering Cancer Center, US and 2021 ASH President, said: “While VWD is
a common bleeding disorder, it is also complex, presenting challenges in the timely diagnosis and appropriate management of bleeding for patients.
“Because diagnosis is not straightforward and symptoms range in severity, there is a need for trustworthy guidelines to
help improve the quality of care for patients.”
Dr Leonard Valentino, President of NHF, added: “These guidelines are an extremely important step in our quest to address the difficulties individuals go through to obtain an accurate, timely diagnosis, and appropriate treatment.“The challenge ahead will be for us to educate both those living with VWD and healthcare professionals on the guideline recommendations.”
The guidelines are accompanied by tools and educational resources to help patients, haematologists and other healthcare providers understand and implement the recommendations. The most common warning sign of VWD for women is heavy menstrual bleeding. One-in-five women will have heavy menstrual bleeding and, of these, up to one-in-five may have an underlying bleeding disorder.
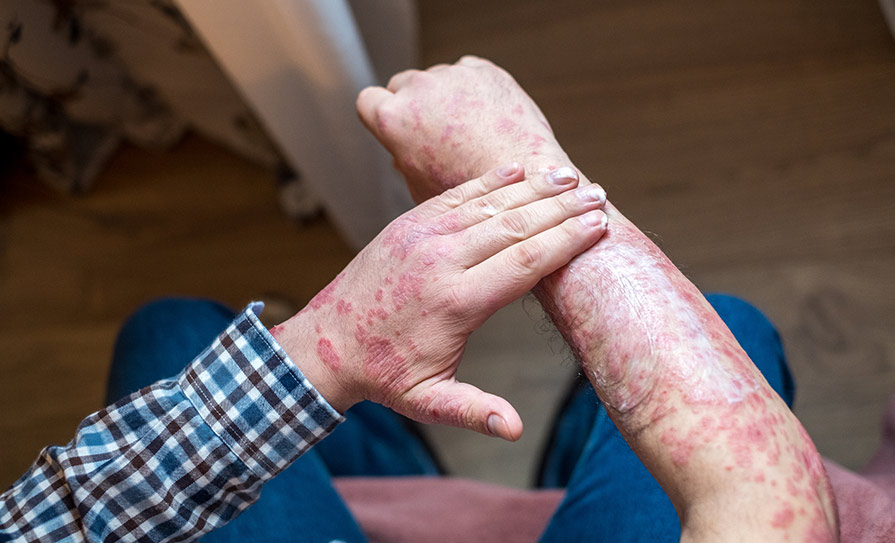
Many people with VWD have suffered through years of frequent nosebleeds, bleeding post dental care, easy bruising or heavy menstrual bleeding prior to diagnosis. There is thus a need to raise awareness among the general public and among GPs that frequent nosebleeds or heavy menstrual bleeding are not normal and may require investigation via referral to a specialist coagulation centre, according to the Irish Haemophilia Society.
Mr Brian O’Mahony, Chief Executive, Irish Haemophilia Society, said: “Von Willebrand disorder is massively underdiagnosed in many countries, including Ireland. There are currently 1,643 people in Ireland diagnosed with VWD of whom 618 are male and 1,025 are female. We would expect to have 4,900 diagnosed if all those with VWD were identified.”
In April, the Society launched a VWD patient information booklet, series of animated and personal videos and host two
webinars to mark World Haemophilia Day. Further information is available at https://haemophilia.ie/







Leave a Reply
You must be logged in to post a comment.