An overview of the presentation and latest treatment approaches to acne vulgaris, with a series of practical cases
Acne vulgaris is a chronic, inflammatory condition of the pilosebaceous unit characterised by inflammatory and non-inflammatory skin lesions. Treatment is directed at the four factors involved in lesion formation which include increased sebum production, hyperkeratinisation of the hair follicle, colonisation by the bacterium Propionibacterium Acnes (P.Acnes), and the resultant inflammatory reaction. It mainly affects 80 per cent of adolescents to varying degrees but is problematic for about 20 per cent with 35 per cent of women and 20 per cent of men having acne in their 30s. It is often overlooked as being a normal occurrence during teenage years. However, acne vulgaris can significantly impact on a person’s quality-of-life, self-esteem and mental health. It is for this reason and also to avoid irreversible scarring, that early treatment is recommended.
During this article, I will discuss the management of the various severities of acne vulgaris and address some commonly asked questions.
Diagnosis
Acne vulgaris is a clinical diagnosis. Closed and open comedones (aka white- and black-heads) are non-inflammatory skin lesions and help differentiate acne vulgaris from other facial rashes such as acne rosacea or a peri-orifical dermatitis.
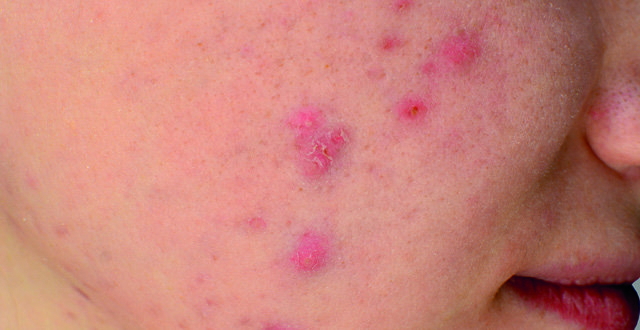
Inflammatory skin lesions include erythematous papules and pustules. These lesions can advance to become nodules or nodulocystic lesions in more severe cases of acne. They can quite often be painful.
It is important to classify a person’s acne into mainly non-inflammatory or inflammatory or mixed as this will help guide treatment.
There are many acne grading scales mentioned in the literature. However, they tend not to be used in clinical practice as they can be cumbersome and time consuming. Acne tends to be graded as mild, moderate or severe. Mild-to-moderate cases consist mainly of comedones, papules and pustules while severe acne vulgaris would also include nodules +/- cysts, sinuses and scarring.
Treatment
Case 1
A 15-year-old boy presents with facial papules, pustules, and some comedones. You have graded his acne as mild and he is not keen on oral medications. How would you treat him?
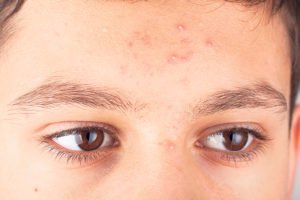
I would manage this patient on topical treatments to target both the inflammatory and non-inflammatory skin lesions. A topical antibiotic such as clindamycin combined with benzoyl peroxide (BPO) should be applied to the inflammatory skin lesions. BPO with a topical retinoid is an alternative approach here. BPO helps to reduce the risk of antibiotic resistance as it is an antimicrobial and works synergistically with the antibiotic. It is the anti-inflammatory quality of antibiotics that help treat these skin lesions. While they do not eradicate the implicated bacterium, P.Acnes, which colonises the pilosebaceous unit, they do reduce the colony count in combination with BPO. You should advise your patients that BPO can bleach materials, eg, clothes, pillow cases, etc, and so it does need to be fully rinsed off.
In addition to the topical clindamycin/BPO combination, I would also prescribe a topical retinoid such as adapalene, which is the best tolerated of all the topical retinoids. This works mainly on the non-inflammatory skin lesions through reducing cell proliferation within the walls of the follicular duct and preventing comedone formation. They are also effective in treating inflammatory skin lesions. People find it difficult to tolerate topical retinoids so it is important to explain to them how it should be applied to ensure compliance. I inform patients that it will dry out their skin, but this is how it works. They should commence applying a half a pea-sized amount every third night to all their spots and to where they would normally get spots. They should continue doing this for two weeks approximately, then increase to once every two nights for a couple of weeks and then to every night if tolerated. If unable to tolerate this, I encourage them to apply it at whatever frequency they can tolerate. Night-time application is recommended as it does render them photosensitive. Data shows that the systemic absorption of topical retinoids is negligible and unlikely to affect the foetus. However, given the high susceptibility of humans to the teratogenicity of oral retinoids, it is advised to avoid topical retinoids if trying to conceive or if pregnant.
It is important to manage patient’s expectations when prescribing topical treatments as they are often disappointed if there is no improvement after a couple of weeks. Patients need to be informed that a potential flare up of their acne within the first two-to-four weeks of their treatment can occur. I tell patients that they should expect a 50 per cent improvement in their skin after two months. It they are not achieving this, I advise them to attend the surgery so that we can re-evaluate their management and potentially increase the potency of it. I think it is reasonable to continue the topical antibiotic/BPO combination for a three-to-four month period. It is recommended to continue topical retinoids following clearance of the acne as they help prevent recurrences. Topical BPO or azelaic acid are other potential options here.
Case 2
The boy in Case 1 returns to you after two months of treatment as outlined above. He is unhappy with the response to treatment. You observe that his acne has worsened in severity with mainly pustules and papules evident. There is no evidence of scarring. How do you manage him?
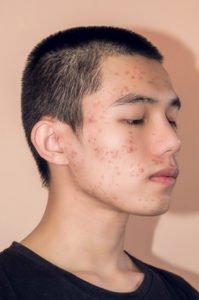
I would stop his topical antibiotic/combination and commence him on a three-month course of oral tetracycline such as doxycycline 100mg OD or Tetralysal (lymecycline) 300mg OD. I would continue the topical retinoid (adapalene) or BPO so as to reduce the risk of antibiotic resistance. I would advise on both the teratogenicity and photosensitivity of tetracyclines. In utero exposure to tetracyclines in the second and third trimester can lead to permanent brown staining of teeth while it is also associated with maternal hepatotoxicity during pregnancy. It is advisable to recommend a non-comedogenic sun factor protection in conjunction with this treatment. Again, I would advise him to attend the surgery in two months’ time if he has not noticed >50 per cent improvement in his skin. Should this occur, I would consider changing to an alternative tetracycline for three months and continue the adapalene. If this patient was female I would also consider adding an oral contraceptive pill (OCP) containing cyproterone acetate.
Case 3
19-year-old girl with moderate-severity acne is looking for both contraception and treatment of her acne. How would you manage this?
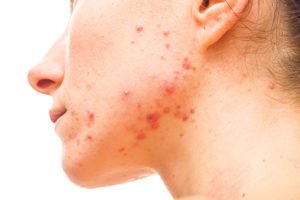
A Cochrane review of oral contraceptive pills (OCPs) demonstrated that the OCPs studied showed improvements in inflammatory and non-inflammatory acne vulgaris. One meta-analysis concluded that while antibiotics may be superior to OCPs at three months, OCPs are equivalent to antibiotics at six months in reducing acne lesions. The OCP can work quite well for patients who report a hormonal type of acne, ie, it flares pre-menstrually, is located along the jawline and is associated with other signs of hyper androgenism such as hirsutism, oligomenorrhoea and a hormonal profile suggestive of polycystic ovarian syndrome (PCOS). Assuming she is UKMEC <3, I would commence her on the OCP containing an anti-androgen, which is the first-line OCP in the treatment of acne. Anti-androgen OCPs include those containing drospirenone (Yasmin) or cyproterone acetate (Dianette). While cyproterone acetate is typically the first-line OCP used in acne, there is no clear evidence outlining superiority of one OCP over another. I tend to prescribe Dianette until the patient’s acne is clear and then aim to change to a less thrombotic OCP, ie, a levonorgestrel-containing OCP, when skin has been clear for four menstrual cycles. However, it is important to mention a Cochrane review of the venous thrombotic events (VTE) of OCPS. It concluded that all OCP use increases the risk of VTE compared to non-users, but is less than the risk associated with pregnancy. The relative risk of VTE for OCPs with 30-35mcg of ethinyl estradiol combined with gestodene (Estelle, Minulet), desogestrel (Marviol, Mercilon), cyproterone acetate (Dianette) or drospirenone (Yasmin) were similar and about 50-to-80 per cent higher than OCPs with levonorgestrel (Microlite, Leonore, Logynon, and Ovranette).
The international Faculty of Sexual and Reproductive Healthcare (FRSH) advise that the non-contraceptive benefits of an OCP containing cyproterone acetate outweigh the risks of thrombosis. Statistically-significant improvements in acne have been noticed after three menstrual cycles. Once this patient’s skin is clear for four menstrual cycles, I would then consider changing her to an alternative OCP, which has a lower thrombotic risk. In conjunction with the OCP I would also prescribe a topical adapalene or BPO to enhance the efficacy of treatment. On clearance of the acne, I would advise that the adapalene be continued to help reduce the recurrence risk.
Case 4
A female patient attends you with mild-to-moderate severity acne vulgaris and informs you that she is 24 weeks pregnant. What can you prescribe?
You could safely prescribe topical azelaic acid, which is Pregnancy Category B, for this lady. It works on both inflammatory and non-inflammatory acne by inhibiting P.Acnes and reducing keratin production within the pilosebaceous unit. To help build up tolerance to it, you can advise your patient to initially apply it once daily and gradually build up to twice daily application. This cream is also useful in managing post inflammatory hyperpigmentation that remains following the successful treatment of acne lesions. This can persist for up to 18 months in Caucasian skin but can be quite troublesome for skin of colour where it can sometimes be permanent.
In moderate to severe acne, oral erythromycin or cephalexin for a few weeks is considered to be safe.
What is oral isotretinoin?
Oral isotretinoin is an oral retinoid and the only potential curative treatment for acne. It works on all the primary causal factors of acne. Treatment courses are typically six months in length. Most people experience a 100 per cent improvement but recurrence rates can vary from 30-70 per cent.
When to consider oral isotretinoin?
It is an excellent option for patients if they meet the criteria for it. This includes:
Severe acne vulgaris.
Moderate severity acne vulgaris that is resistant to treatment or relapses when oral antibiotics or the OCP are stopped.
Moderate severity acne vulgaris that induces psychological stress or results in scarring.
What are the common side effects of oral isotretinoin?
It is usually well tolerated with the most common side effects being dry lips and dry skin. A good moisturiser and lip balm with frequent application can help mitigate against these. Isotretinoin renders the patient more photosensitive so we do advise that patients apply a non-comedogenic sun cream with an SPF of >/=30 and ideally a 5*UVA rating. Rarely, oral isotretinoin can cause a rise in triglycerides or a rise in liver transaminases. To monitor this, blood tests are taken prior to commencing the treatment and one month following initiation.
For some athletes, joint and muscle pains can be an issue. In this instance, a reduction in dosage may help resolve the issue.
In patients with severe acne, they may experience an initial flare of their acne. The risk of this can be reduced by starting with a lower dosage, simultaneously prescribing a course of low dose steroids or extracting some comedones prior to initiation of the oral isotretinoin.
Several early case series described delayed wound healing or keloid formation following isotretinoin usage. Thus, it is recommended to delay procedures such as dermabrasion or laser resurfacing until six-to-12 months following cessation of treatment.
Is oral isotretinoin associated with low mood?
No causative links between oral isotretinoin and low mood or suicidal ideation have been established. Reports to the US Food and Drugs Authority (FDA) have identified an association between the use of this medication and depression with positive de-challenges and re-challenges. Anecdotally, in my own experience, I have found that most patients’ mood remains quite stable or improves as they are quite happy with the response of their skin to treatment. However, I have also seen cases where mood does dip, oftentimes on uptitration of the dosage, but then improves on stopping the medication. In certain instances, the oral isotretinoin has been re-introduced at a lower dosage and the patient has done quite well, but may need a longer course of treatment as a result.
Teratogenicity and oral isotretinoin
Oral isotretinoin is a significantly teratogenic medication. The risk of congenital malformation rises from a baseline population risk of 3-to-5 per cent to 30 per cent among women who undergo exposure during the first trimester. Teratogenic effects include serious craniofacial, cardiovascular, thymic and central nervous system malformations. There is no known teratogenic effect associated with male patients. It is mandatory that female patients (are advised to) use two forms of contraception. Contraception must be commenced one month prior to treatment and continued for one month after treatment has ceased. Pregnancy tests are performed prior to treatment and at monthly intervals thereafter. Despite strict criteria regarding contraception, there are 150 isotretinoin-exposed pregnancies in the US each year, with one study demonstrating non-compliance with barrier contraception in 29 per cent of cases, while 39 per cent missed >/=1 contraceptive pill in the previous month.
Case 5
A patient presents to you with severe acne vulgaris, but is reluctant to try oral isotretinoin. How do you manage?
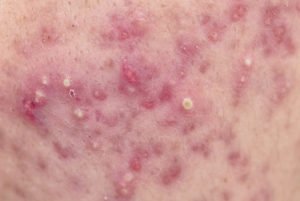
In
this situation, I would recommend a 5 per cent BPO facial rash and prescribe
100mg BD of doxycycline for a maximum of six months with a topical
retinoid.
Tolerability here is key so I always advise patients to take the doxycycline
with food to avoid nausea. If the patient is female, you could also consider
adding in an OCP to augment treatment as we now know that the risk of
contraception failure is not increased by co-prescription with tetracyclines.
Case 6
A 21-year-old female patient presents to your practice and is quite distressed by keloid scarring due to their acne. What treatment ideas can be offered?
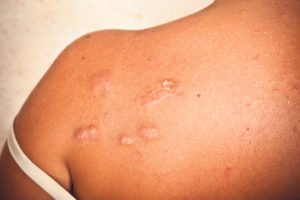
Keloid is one of the common types of scarring in acne vulgaris. Other types include hypertrophic and atrophic scarring including ice pick and boxcar. I offer patients treatment of their keloid and hypertrophic scars. Treatment entails the intradermal injection of 0.1-0.2ml of triamcinolone 10mg/ml per square cm of the scar. It is important for the injection to be intradermal as opposed to subcutaneous so as to avoid excessive dipping/atrophy of the scar. While triamcinolone can work quite well at flattening keloid, the scar itself is irreversible. Other potential treatments of this type of scarring includes clobetasol propionate 0.05 per cent cream under occlusion with a silicone dressing, which has been shown to be as effective as IM triamcinolone injections over a three-month period, but with better tolerability. There are topical silicone gel treatments available over the counter which can be helpful also, with early application being key to a better outcome.
How to reduce the risk of antibiotic resistance?
P.Acnes resistance to antibiotics was first noted amongst acne patients in the late 1970s. Tetracycline and erythromycin resistance levels of 20-30 per cent and 50 per cent, respectively, have been quoted. Resistance leads to a resultant reduction in the effectiveness of treatment.
To try and mitigate against this:
Avoid antibiotic monotherapy. Antibiotics should be co-prescribed with topical adapalene or BPO. These help to enhance penetration of the topical antibiotic while reducing the overall length of treatment.
Do not co-prescribe topical antibiotics with oral antibiotics. There is no benefit to this.
Avoid prolonged courses of oral antibiotics. A complete course is considered to be three months.
Prescribe a topical retinoid as maintenance to help prevent recurrence of acne vulgaris
If your patient is requiring recurrent courses of antibiotics due to quick relapses of treatment, then they should be considered for oral isotretinoin.
Case 7
Parents attend you with their six-week-old baby girl who has an erythematous scaling rash affecting her face with associated pustules and papules. No comedones are present. Cradle cap is visible. The rash is non-pruritic and the baby is not bothered by her rash (but the parents are!). Management?

This is a case which I commonly encounter in general practice. Neonatal acne affects 20 per cent of babies and I often describe it to parents as being ‘cradle cap of the face’ as opposed to acne, which tends to have more negative and long-term connotations for parents. The pathogenesis is different to acne vulgaris. Malassezia furfur is implicated, which explains why a combination cream of miconazole and hydrocortisone works quite well. Applying this cream twice daily usually leads to resolution of the rash after a few days of treatment. It may recur, but the baby tends to outgrow it by three months of age. I advise parents to store this cream in the fridge once opened to avoid loss of efficacy.
References on request












Leave a Reply
You must be logged in to post a comment.