Dr Donna Cosgrove PhD, Pharmacist, takes a clinical look at the diagnosis, impact and treatment of different presentations of psoriasis and how the pharmacist can improve quality of life for these patients
Psoriasis is a multifactorial, chronic, multi-system, inflammatory disease with mainly skin and joint involvement. It can cause itching, irritation, burning, and stinging and typically follows a relapsing and remitting course. In the UK, the prevalence of psoriasis is estimated at around 1.3-to-2.2 per cent. Besides the physical impact, there may also be a pronounced emotional and psychosocial impact on patients, with the disease affecting people’s social lives and interpersonal relationships, even affecting employment and income. Psoriasis, which is a disease of systemic inflammation, is associated with multiple morbidities, ie, cardiovascular disease, lymphoma and melanoma. Psychiatric illnesses, mostly anxiety and depression, also commonly present in up to 60 per cent of patients. Psoriasis affects men and women equally, with most cases occurring before the age of 35 years. It is more common in lighter-skinned than darker-skinned people.
In psoriasis, there is an increased production of skin cells. These are normally made and replaced every three-to-four weeks, but in psoriasis, this process takes about three-to-seven days. The resulting build-up of skin cells creates the characteristic plaques. The process is not fully understood, but the immune system is thought to play a key role. Genetic studies have provided evidence that this is the case, as well as this immune influence being supported by the observation that psoriasis reappears after cessation of systemic corticosteroids, and its lesions are associated with increased T-cell activity in underlying skin.
Psoriasis symptoms can be triggered after a certain event, ie, a skin injury, throat infection, certain medicines like lithium, some antimalarials, ACE inhibitors and ibuprofen. Alcohol, smoking, stress, and hormonal changes can also act as triggers. Most patients report having a family history of psoriasis.
Diagnosis
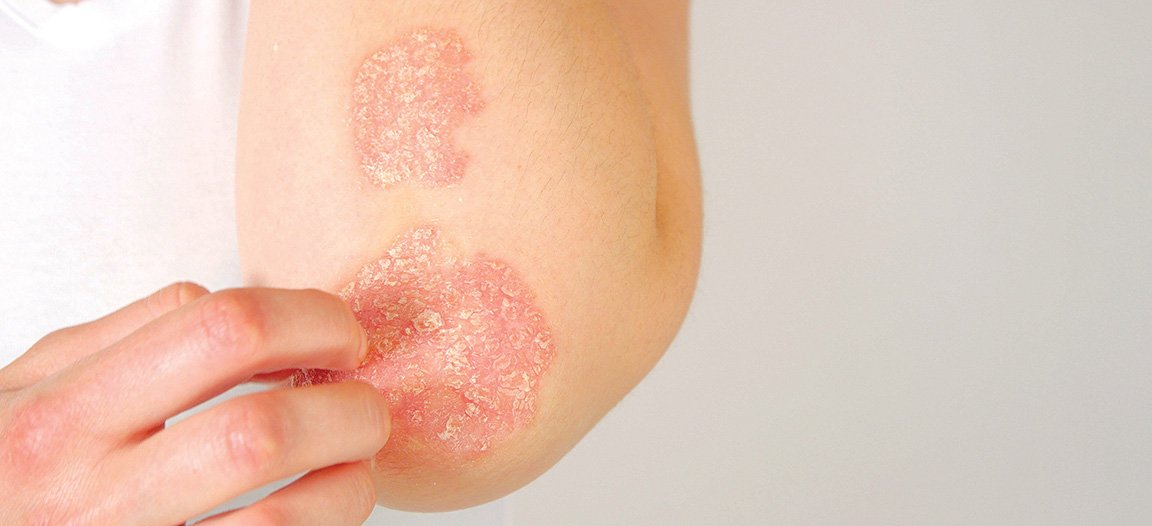
Diagnosis is made clinically, based on the appearance of the skin, although in rare cases a biopsy will be taken to rule out other causes. The most common type is plaque psoriasis, which affects up to 90 per cent of patients with psoriasis. This type is well delineated, symmetric, and features erythematous plaques with overlying silver scale. These are commonly found on the scalp, trunk, buttocks and extremities, but can be found anywhere on the body and can be itchy and/or painful. Nails can also be involved in around 50 per cent of those affected. Psoriasis can cause nails to develop dents or pits, become discoloured, or grow abnormally. They can become loose, separate from the nail bed, or in severe cases, nails may crumble. Nail involvement is more common in those with psoriatic arthritis, which affects approximately 30 per cent of patients with psoriasis. Skin plaques often precede the joint-related part of the disease by a decade. As soon as psoriatic arthritis is suspected, the patient should be referred to a rheumatologist.
When assessing disease severity, NICE guidance recommends using the static Physician’s Global Assessment (clear, nearly clear, mild, moderate, severe, or very severe), asking for the Patient’s Global Assessment (clear, nearly clear, mild, moderate, severe, or very severe), estimating the body surface area affected, checking for systemic upset like fever or malaise, and involvement of the nails or difficult-to-treat sites. The face, flexures, genitalia, scalp, palms and soles are ‘difficult-to-treat’ because psoriasis at these sites may have an especially high impact. In specialist settings, a validated tool, ie, the Psoriasis Area and Severity Index (PASI), should be used to assess severity. There are additional tools available to assess the impact on psychological and social wellbeing, ie, the Dermatology Life Quality Index (DLQI).
Mild psoriasis involves <3 per cent of the body surface area (BSA), has minimal effect on patients’ quality of life (QoL), and is easily managed with routine topical therapy. Moderate psoriasis is between 3 and 10 per cent BSA. This level of psoriasis might not be controlled by routine measures, and/or can substantially affect the patient’s QoL due to the extent, discomfort, or location of the disease. Severe psoriasis involves >10 per cent BSA.
Other types of psoriasis include inverse psoriasis (affects folds or creases in the skin, such as the armpits, groin, between the buttocks and under the breasts); pustular psoriasis (rarer type of psoriasis that causes pustules to appear); guttate psoriasis (small, drop-shaped sores on the chest, arms, legs and scalp); and erythrodermic psoriasis (rare form of psoriasis that can cause intense itching or burning all over, and lead to loss of proteins and fluid). These are less common types of the condition, differentiated from plaque psoriasis by their morphology.
Management and treatment
There is no cure for psoriasis, but multiple effective treatments are available. For mild-to-moderate psoriasis, first-line treatments include topical medications like corticosteroids, vitamin D3 analogues, and combination products. Most people are successfully managed in primary care, but at some stage up to 60 per cent of people will need specialist referral. For the treatment of more severe or refractory symptoms, evaluation by a dermatologist for systemic therapy may be required. NICE guidance recommends traditional topical therapies as first-line treatments, with second-line treatments including phototherapies and systemic non-biologics like methotrexate, ciclosporin, and acitretin. Third-line therapy refers to biologic agents like TNF antagonists (adalimumab, etanercept, infliximab) and ustekinumab, which targets interleukins 12 and 23. Annual assessment should be offered to people with any type of psoriasis. When a new topical treatment is started, a review appointment should be offered after four weeks.
Medications and treatment regimens
Emollients: These moisturising treatments are applied to reduce water loss and cover the skin with a protective film. In mild psoriasis, an emollient is probably the first treatment that should be suggested. The main benefit is reducing itching and scaling. Furthermore, some topical treatments are thought to work better on moisturised skin, however, the patient should wait at least 30 minutes before applying a topical treatment after an emollient.
Corticosteroids: These reduce inflammation, slow keratinocyte turnover and reduce itching. There is still little information available in terms of which corticosteroid works best for psoriasis. A Cochrane review has shown that corticosteroids perform at least as well as vitamin D3 analogues (potent and very potent corticosteroids).
Consider the type of preparations available and suitability for the treatment area, ie, a cream, lotion or gel for widespread psoriasis; lotion, solution or gel for areas with hair; and ointment to treat areas with thick, adherent scale.
The continuous use of potent steroids may cause irreversible skin atrophy and striae, and systemic side-effects may occur when used extensively on the skin (>10 per cent BSA). Ideally, aim for a break of four weeks between courses of treatment, and potent corticosteroids should not be used continuously on any site for >four weeks.
Vitamin D3 analogues: Calcipotriol reduces symptoms by slowing keratinocyte proliferation and by inhibiting T lymphocyte activity. It has been shown to be safe and efficacious in mild plaque psoriasis, and not inferior to corticosteroids.
Combination products: Products containing calcipotriol and betamethasone are more effective for plaque psoriasis than either on its own.
Calcineurin inhibitors: Tacrolimus or pimecrolimus preparations reduce inflammation. These medications are used in some cases when steroid creams are not effective in sensitive areas such as the scalp, flexures, and genitals.
Coal tar: Tar can help slow the rapid growth of skin cells and restore the skin’s appearance.
Dithranol: This has been used for more than 50 years in the treatment of psoriasis. It slows the production of cells. It is usually applied to the skin for up to an hour and then washed off.
Phototherapy: This is useful in guttate psoriasis and moderate or severe plaque psoriasis unresponsive to topical agents. UVB phototherapy is usually offered two-to-three times a week.
Methotrexate: Systemic non-biological therapy should be offered when topical treatments and phototherapy do not help, or if there is a significant impact on physical, psychological or social wellbeing, or in otherwise severe cases. This is an inhibitor of folate synthesis with cytostatic and anti-inflammatory properties. Even now, there are not many studies that evaluate methotrexate efficacy in psoriasis, but one study reports a 75 per cent improvement in PASI score in almost 40 per cent of patients compared with 18.9 per cent on placebo after 16 weeks. Side-effects such as hepatotoxicity do occur. LFTs should be performed before and during methotrexate therapy.
Cyclosporin: This calcineurin inhibitor is used for psoriasis and psoriatic arthritis. It has a rapid onset of action and brings less concern about myelosuppression or hepatotoxicity, but it brings its own potential adverse effects, including nephrotoxicity and hypertension.
Acitretin: This is an oral retinoid that reduces skin cell production. Acitretin has a wide range of side-effects, including dryness and cracking of the lips, dryness of the nasal passages and, in rarer cases, hepatitis.
Biologic therapy: If the psoriasis does not respond to the first choice of biologic drug (infliximab — within 10 weeks; etanercept — 12 weeks; adalimumab, ustekinumab — 10 weeks), consider changing to an alternative biologic. Other first-line treatment options for psoriasis include secukinumab, ixekizumab, guselkumab, brodalumab, certolizumab pegol, tildrakizumab, and risankizumab. Choice of first-line treatment will depend on the severity and type of psoriasis.
Apremilast and dimethyl fumarate are newer medicines that reduce inflammation. These are only recommended in severe psoriasis that has not responded to other treatments, such as the biological treatments.
Trunk and limbs: NICE guidance recommends a potent corticosteroid applied once daily plus a vitamin D/vitamin D analogue applied once daily, separately (one morning, one evening) for up to four weeks as initial treatment for adults with trunk/limb psoriasis.
If this does not work, a vitamin D/vitamin D analogue can be tried alone twice daily. If this is unsuccessful, application of a potent corticosteroid twice daily can be tried, or use of a coal tar preparation once or twice daily. Very potent corticosteroids are used in specialist settings, or when other topical treatments have not worked, and for a maximum of four weeks. Short-contact dithranol can be considered for treatment-resistant psoriasis of the trunk.
To treat psoriasis on the scalp, a potent steroid applied once daily for four weeks is the initial choice.
For the face, flexures, and genitalia, a short-term mild- or moderate-potency corticosteroid once or twice daily is the first-line treatment. However, these areas are particularly vulnerable to steroid atrophy and should be used at a maximum for one-to-two weeks per month.
For patients who need systemic therapy, methotrexate is first-line, unless rapid or short-term disease control is required, or conception is being considered and systemic therapy cannot be avoided. In these cases, ciclosporin is a better choice. If a patient is not responding to one of these, the other can be tried. Acitretin can be considered if methotrexate and ciclosporin are not appropriate or have not worked.
Support
People being treated for psoriasis should be offered support and information to suit their individual needs so that they can confidently understand their diagnosis, treatment options, risk factors and how to use their medication, and should be given strategies to deal with their psychological wellbeing. Treatment strategies that minimise the impact of their condition should be developed, with assessment tools used to measure this. The risks and benefits of treatment options should be discussed as appropriate. Practicing good ‘self-care’ is also important for people with psoriasis. This includes staying fit, maintaining good physical and mental health, preventing illness or accidents, and caring more effectively for minor illnesses and long-term conditions. People with long-term conditions like psoriasis can benefit enormously from self-care. It improves mortality, decreases pain levels, reduces the risk of anxiety, depression and fatigue, and provides a better quality of life.
References on request
ISF Dermatology Study Day 2020
The Irish Skin Foundation’s (ISF) fifth annual Dermatology Study Day will take place on Saturday, 21 March in the Ashling Hotel, Parkgate Street, Arran Quay, Dublin 8 from 9am–3:20pm.
Delegates can look forward to an interesting line up of expert speakers from the world of dermatology. The 2020 programme is designed for hospital, community-based, GP practice, public health nurses, pharmacists and others involved in providing first-line management of skin conditions/diseases. The programme will cover: Skin infections; melanoma; rosacea, acne and scarring; psoriasis; chronic itch; blistering skin disorders; and wound management.
The annual event provides an exciting opportunity to learn from the experts and bring new knowledge and skills back to the workplace. Attendees will also get the opportunity to meet and talk during the event with exhibitors on new and innovative products on the market.
The 2020 programme includes:
09:00-09:25 Registration & tea/coffee
09:25-09:30 Opening and welcome address
Carmel Blake, Dermatology ANP at Tallaght University Hospital, ISF Helpline
Clinical Manager
09:30-10:10 An overview of common skin infections
Dr Maeve McAleer, Consultant Dermatologist
10:10-10:50 Assessment and management of melanoma
Dr Shirley Potter, Consultant Plastic, Reconstructive and Aesthetic
Surgeon
10:50-11:30 “Does she need another joule?” Acne, rosacea and lasers
Dr Rosemary Coleman, Consultant Dermatologist
11:30-12:00 Tea/coffee break
12:00-12:40 Up-to-date management and treatment of psoriasis
Prof Anne-Marie Tobin, Consultant Dermatologist
12:40-13:20 Chronic itch: causes and treatments
Dr Ian McDonald, Dermatology Specialist Registrar
13:20-14:00 Complimentary Lunch & Exhibition Stands
14:00-14:40 Identifying and understanding blistering skin disorders
Sheila Ryan, Dermatology Advanced Nurse Practitioner
14:40-15:20 Practical approaches to wound management
Gillian O’Brien, Dermatology Advanced Nurse Practitioner
15:20 Ends
The ISF Dermatology Study Day 2020 promises to be an unmissable event, so we advise people to get their ticket well in advance to avoid disappointment.
Registration Fee: €75 including tea/coffee breaks and lunch. CPD points from Irish College of General Practitioners (ICGP) and the Nursing and Midwifery Board of Ireland (NMBI) approval is pending.
Tickets can be downloaded from Eventbrite:
www.eventbrite.ie/e/isf-dermatology-study-day-
2020-tickets-91154297959
For further Information on the Irish Skin Foundation please visit www.irishskin.ie












Leave a Reply
You must be logged in to post a comment.