Dr Niall F Davis provides a comprehensive overview on iatrogenic complications, indications, technique and future perspectives in catheter-related technologies
Urethral catheterisation (UC) is routinely performed in hospital and community settings, with ≤25 per cent of hospitalised patients catheterised during their inpatient stay. All newly-qualified doctors are expected to be safe, confident, and competent at performing UC at the end of their training. Complications related to the placement and management of urinary catheters are a significant source of patient morbidity. Common complications of urinary catheters include catheter-associated urinary tract infections (CAUTIs), non-infectious complications, and device malfunction.
CAUTIs are one of the most common healthcare-associated infections, accounting for 34 per cent of hospital-acquired infections and approximately 76 per cent of urinary tract infections (UTIs) are associated with the use of catheters.
In contrast, catheter-related trauma receives less attention, even though catheter-related trauma increases the chances of developing infection and other associated complications. Notably, studies demonstrate that urinary catheter-related trauma is as common, if not more common, than urinary CAUTIs. Traumatic UC is associated with increased morbidity, increased length of inpatient stay, resource utilisation and even surgical intervention. Long-term morbidity can include urethral stricture disease, urinary incontinence and erectile dysfunction. Traumatic catheterisation may also result in more serious complications, such as acute kidney injury requiring intensive care admission, urosepsis, blood transfusions, and increased hospital costs. Addressing the issue of traumatic catheterisation is important so that clinicians can develop approaches to decrease the incidence, and quality improvement efforts should continue to focus on reducing the incidence of non- infectious complications.
Evolution of the urinary catheter
There is an unmet clinical need to devise, construct, and introduce safer urinary catheters with protective safety mechanisms. At present, the most widely-used urethral catheter was devised by Foley in 1929 and its design was finalised and patented in 1936. Until recently, no significant modification has occurred for improving the safety profile of urinary catheters. The modern Foley catheter (1980s) is coated with a silicone elastomer to reduce latex toxicity of the original device. Catheter research in the last few years has largely focused on reducing UTIs by coating antiseptic or antimicrobial agents over the catheter.
Urinary catheters differ in terms of their sizes, design, and constituents. The sizes of current urinary catheters range from 3.5 to 40 French and the most commonly-deployed urinary catheters are between 16 and 18 French. Catheters also vary in their material and are composed of latex, Teflon-coated, antimicrobial-coated, and silicone.
As technological advancements are developed, it is likely the design of the urinary catheter will continue to evolve. The introduction of three-way catheters facilitated continuous bladder drainage and irrigation in patients with visible haematuria. The coude catheter (with a curved tip) was developed for placement in male patients with a high bladder neck or to bypass an upward curvature between the bulbar urethra and prostatic urethra.
Training modules
Male urethral catheterisation can be more challenging than female due to urethral length, more torturous urethra and an enlarged prostate. Education programmes are helpful for inexperienced healthcare professionals but are not compulsory or failsafe and successful UC remains operator-dependent. Current methods for catheter-related training and examination of skill acquisition are largely simulation-based. Simulation-based training suits all learning types and helps in better attainment and retention of procedural skills; however, one Irish study on UC reported that 76 per cent of interns felt their practical training for UC was non-existent or inadequate and 52 per cent did not receive any supervision during their first UC. There is also significantly higher UC-related morbidity caused by newly-qualified interns (July to January) compared to interns in their last six months of training (January to July).
Furthermore, this lack of confidence and insufficient experience among junior doctors is reflected by the fact that one-in-five first-year UK interns had never performed male catheterisation and nearly half (45 per cent) had never performed a female catheterisation after one year of medical practice. A lack of continuous training and regular inspection of procedural skills among experienced healthcare staff may be plausible explanations. Urinary catheterisation is also regularly performed by nursing staff and community health nurses, however educational materials to train nurses in catheterisation can be incomplete or may contain inadequate information.
Indications and contra-indications for urinary catheterisation
The following is a list of the most frequent indications for inserting a urinary catheter:
Urinary retention.
Urine output monitoring.
Collection of a sterile urine specimen for diagnostic purposes.
Nerve-related bladder dysfunction (ie, spinal trauma, intractable incontinence).
Imaging study of the lower urinary tract.
Advice should be sought in the following scenarios prior to inserting a urinary catheter — pelvic or perineal trauma associated with perineal bruising and swelling and/or blood at the meatus; and patients with a history of urethral stricture disease or difficult catheterisation.
Correct
technique for
urinary catheter insertion
The standard sterile technique for inserting a urinary catheter involves the following sequence of steps:
Introduce yourself and consent the patient on what you are about to do and the indication for catheterisation.
Wash your hands, ensure you have properly identified the patient and that they have no known drug allergies (ie, lignocaine gel).
Ensure that you have a catheter kit prepared.
Put on sterile gloves and drape the patient. Begin by placing a sterile cover drape with a hole that is centred around the patient’s external genitalia.
With your non-dominant hand, separate the labia in a female or place the penis on slight stretch in a male.
With your dominant hand, clean the urethral meatus with an antiseptic cleaning agent.
Take the tube of local anaesthetic/lubricant and instil the solution into the urethral meatus. Afterwards, advance the tip of the catheter into the urethral meatus down the urethra.
Advance the catheter by grasping it near the urethral meatus and passing it gently and slowly until urine drains. There may be some resistance at the level of the membranous urethra or prostate gland that can usually be managed by slow, steady pressure on the catheter. Do not force the catheter if it will not pass easily.
Never inflate the catheter balloon until you have confirmation that urine is draining from the catheter’s drainage port.
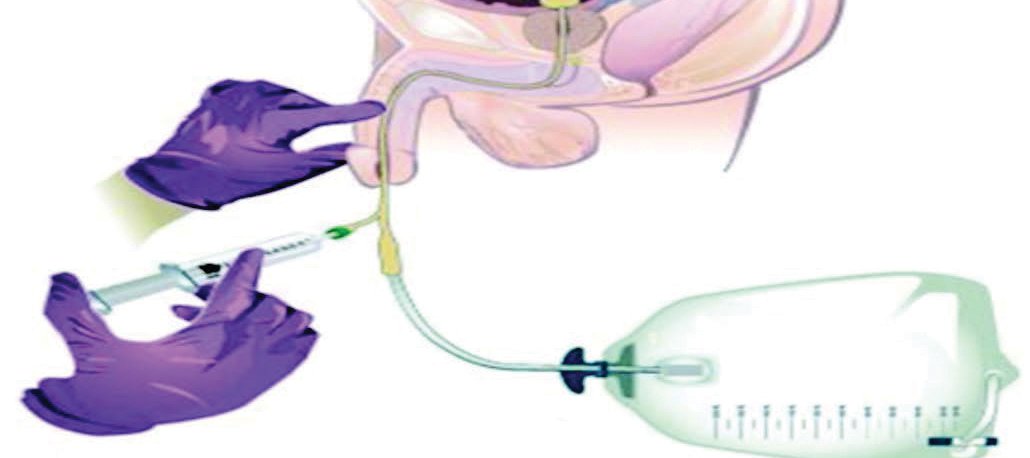
Inflate the catheter balloon with sterile water (10ml) (Figure 1).
Secure the catheter to the patient’s leg and replace the foreskin in an uncircumcised male.
Urethral strictures, bladder neck contractures, benign prostatic hyperplasia, poor technique, false passages, phimosis, meatal stenosis and prostate cancer are some underling coexistent morbidities that can lead to difficult catheterisation.
Complications associated with urinary catheterisation
Improper catheterisation can lead to urethral injury, with devastating long-term clinical sequelae. Urethral trauma may occur due to creating an iatrogenic false passage during catheter insertion or due to inflation of the anchoring balloon in the urethra. Although seldom life-threatening, iatrogenic urethral injury associated with catheter insertion may lead to urethral stricture disease in ≤80 per cent of cases. Benign prostatic hyperplasia is associated with difficult catheter insertion and a consequently greater incidence of urethral injury.
In summary, a misplaced anchoring balloon can result in the following complications:
Urethral trauma.
Urethral rupture.
Urinary retention.
UTIs.
Septicaemia.
Urethral stricture.
How to prevent catheter trauma
Educational programmes
Although technological alterations of basic catheter mechanics will likely result in an incremental decrease in catheter-related trauma, education on the proper catheterisation technique is probably the first and most important step toward successful avoidance of injury. This is not an easy task as, unlike any other medical procedure, most levels of healthcare providers, from nursing to medical students to physicians, routinely insert urinary catheters. All healthcare professionals should be targeted for educational programmes in contemporary practice, since historical data has demonstrated that ≤40 per cent of nurses and junior doctors in academic settings may not know the proper technique of urethral catheterisation.
Kashefi et al were among the first to report the importance of nursing education in preventing iatrogenic urethral injury. In their study, the number of iatrogenic urethral catheter injuries were monitored before and after the commencement of a nursing education programme. After comparing data from a six-month period, the authors noted a 4.9-fold decrease in urethral injuries in the post-education phase of the study. At many academic centres, when nurses have difficulty with catheter placement, the first person asked to aid is the intern. However, in one assessment of intern preparedness for urethral catheterisation in Ireland, Thomas et al reported that 76 per cent of interns believed that their practical training was non-existent or inadequate. In this large retrospective series, most of the injuries resulted from interns performing urethral catheterisations within the first six months of training. Clearly, adequate instruction of medical students and junior physicians on the proper technique of urethral catheterisation should be compulsory to further prevent any iatrogenic injury.
Technological advances
Despite extensive efforts to educate healthcare professionals, it is likely that urethral injuries will continue to occur, since training such a wide variety of healthcare professionals and assessing competence pose significant practical challenges. The introduction of catheter safety mechanisms could potentially prevent injury related to inadvertent balloon inflation in the urethra, thereby reducing iatrogenic catheter morbidity and financial penalties.
Current catheter design lacks inherent safety mechanisms for preventing balloon inflation injury. We reported on safer UC with utilisation of a ‘prototype safety-valve’ that allowed fluid within the syringe to decant through an activated safety threshold pressure valve. The intrinsic threshold inflation pressure for activating this safety prototype syringe pressure valve was 153 kPa, compared to maximum pressure of 452 kPa with a standard syringe. Introduction of such safety mechanisms could potentially prevent injury related to inadvertent balloon inflation in the urethra.
Conclusions
Traumatic catheterisation is preventable, under-reported and relatively common in clinical practice. Importantly, most traumatic catheterisations lead to significant morbidity and are often the result of improper education techniques. Training in urethral catheterisation should be universal, standardised and should be designed to include step-by-step instruction. During the catheterisation process, it is imperative to remember important factors such as history-taking so that the potential for underlying comorbidities (ie, benign prostatic hyperplasia) associated with increased risk of urethral injury can be identified.
Given the risk of serious patient injury, training should be delivered by urologists prior to the beginning of internship when junior doctors and/or nurses are in regular clinical contact with patients. In addition to educational initiatives, we must be willing to advocate for urethral catheter design modifications to eliminate the risk of catheter injury due to operator error.
References on request












Leave a Reply
You must be logged in to post a comment.