Attendees at UCD’s Charles Institute Seminar Series heard a presentation by Prof Xiaoli Wu on treatment considerations for keloid lesions, an under-recognised medical condition.
The Charles Institute, Ireland’s national dermatology research and education centre, hosts a range of guest speakers who cover a variety of topics ranging from skin cancer to psoriasis, among many others. The series, which is sponsored by RELIFE (part of the A.Menarini group), is designed to provide expert advice from a range of distinguished national and international experts in their respective fields and is chaired by Prof Desmond Tobin, Full Professor of Dermatological Science at UCD School of Medicine and Director of the Charles Institute of Dermatology. The seminars are broadcast to attendees with a special interest in dermatology and cutaneous science in other locations, who access the talks remotely via an audio-visual link.

The seminars are held using a hybrid model, combining in-person attendance with interactive online access.
Attendees heard a presentation by Prof Xiaoli Wu, head of the Scar Treatment Team in the Plastic Surgery Department at Shanghai Jiaotong University School of Medicine, China, where she specialises in the treatment of keloid disease and all kinds of scars. Among other distinctions, Prof Wu is Vice-Chair of the Committee on Scar Medicine with the Chinese Association of Plastics and Aesthetics, and Chair of the Scar Group in the Committee on Repair and Reconstructive Surgery in the Chinese Association of Rehabilitation Medicine. Prof Wu is also Chief Editor of the influential Practical Techniques of Scar Treatment, which was published in February of this year, and she plays a pivotal role in several important scarring groups within the Chinese Medical Association.
Prof Wu delivered a presentation titled ‘Keloid Disease – A Neglected Medical Problem’. She explained that keloid disorder represent a fibroproliferative disorder that can cause significant disfigurement and impact severely on a patient’s quality of life. Physicians are familiar with the traditional methods of treating these lesions, which include laser therapy, injections, and surgery, among others, but each of these treatments on its own risk of keloid recurrence. Prof Wu discussed more comprehensive therapy that is focused on managing different medical interventions, depending on the subjective and objective circumstances of the keloid patients. She described different comprehensive strategies based on her clinical experience. One of these is the laser therapy approach, combined with radiotherapy, which Prof Wu described as “a promising method, especially for keloid lesions and wide-based pathological scars”.
Abnormal scar
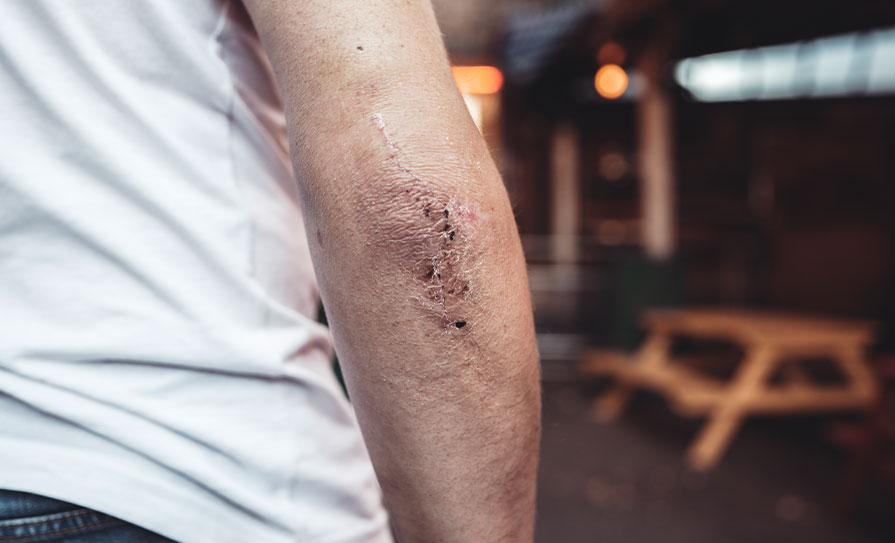
In basic terms, a keloid lesion is abnormal scar tissue formed after skin wound-healing or skin injury healing due to unknown causes that rises above the skin’s surface, with a hard texture and poor elasticity, and which may be accompanied by itching and/ or pain. There are a number of differential diagnoses, including dermatofibrosarcoma protruberans, hamartoma, leiomyosarcoma, spindled-cell tumours, skin cancer, low-grade myofibroblast sarcoma, peripheral nerve sheath tumour, or artificial dermatitis, as well as some other skin diseases. The treatment objectives are symptom improvement with relief from itching and pain, reduced scar volume, prevention of recurrence, and an overall improvement in quality-of-life. Treatment approaches vary from steroid injection to radiotherapy or surgery, among others.
Prof Wu presented case studies illustrating different types of keloid lesions and explained how one keloid lesion can be cured in a patient, but other lesions subsequently appear over a number of years due to the inflammatory state in the body, which makes the lesions difficult to treat. The case studies covered patients of different ages, with different keloid lesions manifestations.
Keloid disorder lesions grow aggressively, and the pathogenesis and mechanism are still unknown
She stressed the need for a comprehensive treatment plan that incorporates medicine, adjuvant therapy, surgery, and laser interventions. In such a plan, treatment with medicine could include the use of oral or external medicine, or steroid injections. Surgical options include total resection, intralesional excision or excision of the lesion’s core, whilst laser interventions could involve an approach using pulsed dye laser (PDL), intense pulsed light (IPL), or ablative laser therapy. Adjuvant interventions can include dietary strategies and/or traditional Chinese medicine, she said.
Comprehensive treatment
Regarding comprehensive surgical treatment, “the indications include a tumour keloid lesion, multiple keloid lesions, keloid lesions that frequently become infected, and if they interfere with a person’s functioning,” Prof Wu said. “Contraindications are if there is systemic disease, if the patient is a child, if there are large areas of inflammatory keloid, if the patient has a mental disorder, and if they are unable to return regularly for a review or are non-compliant.” In a surgical procedure, it is important to thoroughly remove the infection and avoid creating extra wounds, she pointed out. It is also important to use a tension-reduced suture, to staunch the bleeding and close the cavity, and to promote primary healing.
Glucocorticoid injection therapy has the advantages of being non-surgical and inexpensive, with a precise effect, said Prof Wu. However, the disadvantages include some side-effects, the fact that it may be necessary to administer the injections over a longer period of time, and the possibility of recurrence, she added.
“Steroid injection therapy can be indicated if there is an obvious inflammatory effect, if it is a new lesion, if a small area is infected, or if the lesion is on an area that is visibly important,” Prof Wu told the seminar. “The contraindications include if there is pregnancy and lactation, if it is a giant, cauliflower-like keloid lesion, and if there are multiple areas affected. It is also contraindicated in children and the elderly or infirm, if the patient also has a major disease, or if there are dense, multiple areas of keloid. The patient may also have an allergy to steroids,” she added.
She also briefly described the benefits of PDL and IPL laser treatments, which have the effect of reducing redness, and C02 laser or micro-plasma, which has the advantage of reducing tissue volume.
Prof Wu also discussed a new treatment method – laser combined with radiotherapy (LCR), which can be an effective intervention when used on the right patient. “The indications include obviously inflammatory disease, relatively flat keloid lesions whose thickness <5mm, and if the lesion is not close to the thyroid gland or breast,” she told the attendees. “Contraindications are if the patient has systemic disease, has mental or psychological problems, if they are pregnant or lactating, in cases of planned parenthood, or if there is a giant, cauliflower-like lesions,” she said. “This procedure is also contraindicated in children.”
“Keloid disorder lesions grow aggressively, and the pathogenesis and mechanism are still unknown,” said Prof Wu. “There are many different treatment methods, but the recurrence following each treatment method is very high.
“It is not just a depressing condition for patients, but doctors also,” she concluded. “There are many existing treatment methods aimed at local lesions, but not at the systemic condition.” She also observed that there is currently no specific, consistent treatment worldwide for the condition and there is difficulty studying this illness because it only occurs in humans, and not in animals. “We need to find the pathogenesis of this disease and we need to find therapeutic targets to develop targeted drugs.
“Keloid disease is a depressing illness and requires doctors and patients to build confidence together,” Prof Wu continued. “We need to adopt sequential, accurate and three-dimensional treatment strategies and to avoid irregular treatment, LCR may become a powerful weapon for the treatment of thin keloid lesions.”
Acne lesions
During a lively Q&A interactive session and clinical discussion following the presentation, Prof Tobin commented on the wide range of keloid disorders discussed in Prof Wu’s talk. He also noted the Seminar’s value as a comprehensive clinical overview of a condition with a wide variation in phenotypes. With regard to acne lesions, he asked: “You indicated that acne lesions can lead to keloid lesions. You also mentioned the high risk of infection in the keloid disorder. Does that infection originate internally, or does it come from external sources – in other words, does the barrier of the acne lesion to keloid break down?”
Prof Wu commented: “When acne is growing, the bacteria in the acne can stimulate the skin to develop keloid lesions,” she said. “When the keloid lesions grows bigger and bigger, some part of the hair follicle and bacteria can affect the skin, and this can be the source of additional infection.”
Prof Tobin also asked about the influence of family history in the development of keloid disorder. “This disease certainly has some genetic component,” Prof Wu responded. “While a person may have systemic keloid disease, their parents or other close relatives may have no keloid disorder at all. Sometimes, a relative may have several keloid lesions, but their children may have no keloid disorder at all.” For this reason, establishing a family history of keloids is a little difficult, she concluded.










Leave a Reply
You must be logged in to post a comment.