Eczema is a far more debilitating condition than often portrayed with multiple negative impacts on patients and caregivers, thus its burden should not be underestimated, the recent 2022 Primary Care Dermatology Society of Ireland (PCDSI) Annual Meeting heard.
Eczema is the most common persistent inflammatory disease of early childhood; 60 per cent of cases begin during the first year of life while 85 per cent begin before five years.
Dr Maeve McAleer, Consultant Dermatologist, St James’s Hospital, Dublin, and Children’s Health Ireland, and noted researcher in paediatric eczema, gave a comprehensive talk on the presentation, aetiology, impact, and treatment of eczema (aka atopic dermatitis) at the PCDSI meeting.
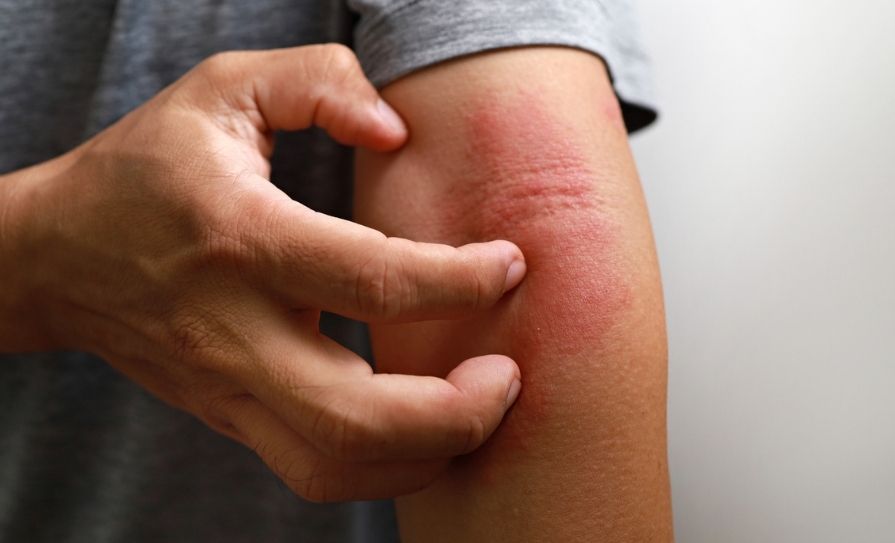
Atopic eczema causes a dry, red, itchy rash; it may be scaly, weep, bleed or crust over, and the condition affects one-in-five children and one-in-10 adults. The hallmarks are intense itch, associated discomfort and pain, and skin inflammation. These symptoms interfere with sleep, the ability to perform day-to-day activities, school performance, ability to work, and are associated with social stigmatisation, Dr McAleer noted.
She highlighted a number of studies showing the significant impact of eczema on children and their families, and also touched upon some of the longer-term health (cardiovascular and psychiatric) risks of eczema.
One of the key building blocks of a healthy skin barrier is a protein called filaggrin, which is defective in patients with eczema, Dr McAleer explained, adding that two-thirds of eczema patients have one or more filaggrin mutations.
Disease triggers in eczema include climate, irritants (wool/rough fabrics, detergents, and fabric softeners, etc), environmental and food allergens, while patients with eczema are more susceptible to superimposed cutaneous infections (staph aureus, chicken pox, warts, etc). Eczema in babies often starts on the cheeks and is frequently associated with food allergy.
A general approach to first-line management of eczema includes (detailed) patient education, daily bathing, emollient use, appropriate strength topical corticosteroid use, and treatment of any complicating infection, she outlined.
Dr McAleer said emollients should be used once to twice daily, be free of dyes, fragrances, and food-derived allergens, and she advised decanting with a spoon to avoid recurrent infection risk.
She noted that aqueous cream has been shown to irritate the skin of both healthy subjects and those with eczema, yet it remains the most commonly-prescribed emollient in the UK.
Discussing once-daily topical corticosteroids, Dr McAleer recommended the use of ointments over creams, as they have a higher concentration of lipids, less preservative, and increased efficacy. The potency should be tailored to the individual’s eczema severity and body site, with a proactive (rather than reactive) approach taken, using daily moisturising and a mild-to-moderate steroid intermittently, with a step-up treatment approach of seven-to-14 days for flares.
Oral JAK inhibitors are being shown to have a positive impact, with a rapid onset and high rate of efficacy, on more severe disease, but longer-term studies are needed to determine their risk benefit profile, she concluded.
A recent major research study co-authored by Dr McAleer, and published in the British Journal of Dermatology, offers hope for the improved treatment of infants with eczema. The research showed that corticosteroid treatments reduced disease severity and normalised immune dysregulation.
Increased local and systemic inflammation is evident in infants with eczema, but it is not clear what effect standard treatment with topical corticosteroids has on inflammation within this patient group.
In the study, a team led by Dr McAleer and Prof Alan Irvine from Trinity’s School of Medicine, set out to investigate responses to first-line corticosteroid treatments in infants with eczema and examine the effect of corticosteroid therapy on skin and blood biomarkers of inflammation.
They recruited 74 treatment infants (<12 months of age) with moderate to severe eczema, through the atopic dermatitis clinic at Children’s Health Ireland, Crumlin. Using minimally invasive skin tape stripping, skin samples were collected before and after a six-week course of treatment with topical corticosteroids. Blood samples were also collected at both time points.
The team found that topical corticosteroid therapy led to an improvement in disease severity, but treatment also normalised systemic immune dysregulation in infants with eczema. Following treatment, altered skin and blood cytokine profiles approached levels seen in children without eczema. Moreover, the results suggest that local inflammation within the skin is responsible for immune dysregulation in infants with eczema.











Leave a Reply
You must be logged in to post a comment.